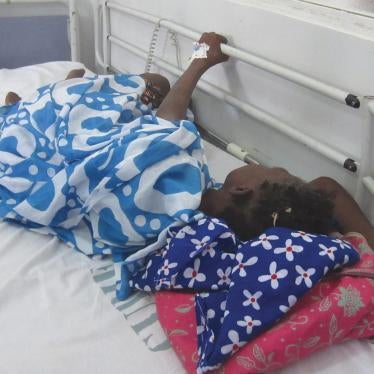
“I am in pain 24 hours a day”, Mamadou* told a Human Rights Watch researcher. “The pain I have all over my body…it is in my bones.”
Mamadou, a 47-year-old man from rural Senegal, has advanced prostate cancer that has spread throughout his body. He can no longer be cured, but with morphine, a strong painkiller, he could live his last months in dignity. However, morphine is hard to get in Senegal, as it is in much of Africa, and supplies are unreliable. During the interview, Mamadou struggled even to speak. “I cannot have a real life without my medication”, he said.
Still in pain
Mamadou is not alone in his suffering. Millions of patients in Africa with advanced cancer, HIV or other illnesses live and die in extreme pain every year. And their numbers grow year by year. In 2007, there were over 700,000 new cancer cases and nearly 600,000 cancer-related deaths in Africa, though those figures do not include the many people who are misdiagnosed or never diagnosed at all. Non-communicable diseases are expected to become Africa’s biggest killer by 2030, surpassing maternal, child and infectious diseases.
But much of the suffering Mamadou and so many others face could be addressed. Palliative care, a health service that focuses on improving the quality of life of patients with incurable illnesses, is highly effective in treating debilitating symptoms, including severe cancer pain. Moreover, it can be provided at relatively low cost, making it realistic to provide this health service even when resources are tight. The World Health Organization has encouraged all countries to ensure that palliative care is integrated into public healthcare systems.
Yet, palliative care services do not exist in almost half of Africa’s countries. In most others, they are accessible to only a small percentage of patients who need them. As a result, many patients die in their homes, in agony and without proper support. For example, in Senegal, palliative care is only available in the capital Dakar – and even there it is very limited. According to the International Narcotics Control Board, in many African countries, morphine is simply not available, even though it is inexpensive and essential for treating severe cancer pain.
Hope on the horizon
But there are positive signs that African leaders have heard the cries of those who suffer. At a meeting in Ethiopia’s capital Addis Ababa last month, African Union health ministers recommended that member-states integrate palliative care into national strategies to combat non-communicable diseases. They also adopted a progressive common position on improving access to strong pain medications that calls for efforts to drastically increase their availability for patients. These initiatives have the potential of leading to vastly improved care for patients with incurable illnesses and their families.
It is also encouraging that Africa already has several excellent palliative care models that other countries can use or adapt. In Uganda, for example, the government has worked closely with palliative care advocates and the healthcare system to develop home-based palliative care services and provide free access to oral morphine. The government and Hospice Africa Uganda are training palliative care specialists, and legal changes have been made to allow appropriately trained nurses to prescribe oral morphine to patients in pain.
In Kenya meanwhile, the government has worked with the Kenyan Hospice and Palliative Care Association to integrate palliative care into 44 public hospitals and to train healthcare providers. Last month, the Health Ministry announced that it was going to supply morphine through the Kenya Medical Supply Agency (KEMSA) to all public hospitals that are providing palliative care.
Progress has also been made in countries as diverse as Zimbabwe, Rwanda, Swaziland, Mozambique and Nigeria, often in cooperation with the African Palliative Care Association. But much remains to be done. As African leaders celebrate the 50th anniversary of the Organization of African Unity/African Union, they have an opportunity to take action to ensure that people like Mamadou do not have to suffer unnecessarily.
African leaders at the summit should set the ball rolling by adopting the recommendations of health ministers. Considering the fact that populations in Africa are aging and that the prevalence of chronic diseases is increasingly rapidly, African leaders would also be addressing a great need that the African Union will face in its next 50 years.
*Names have been changed.
Emmanuel Luyirika is the Executive Director of the African Palliative Care Association and Claude Moreira is President of the Association Senegalaise des Soins Paliatifs.