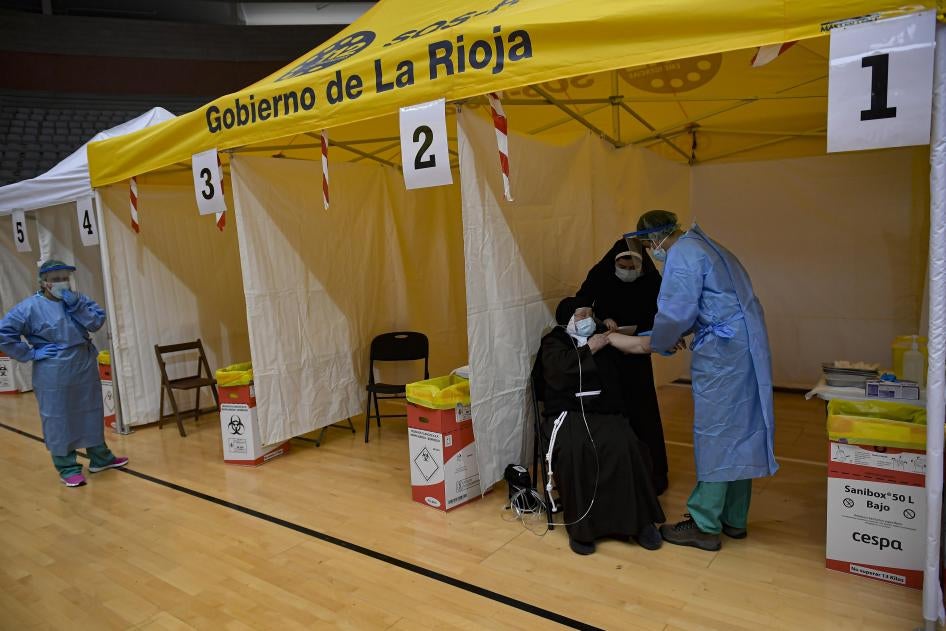
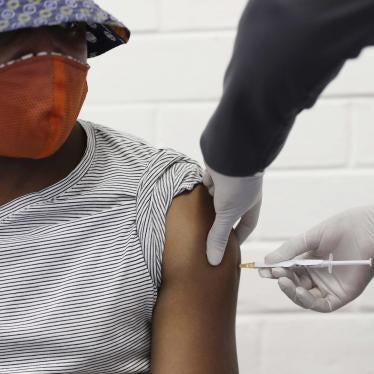
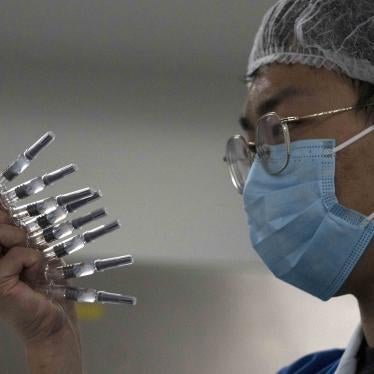
Each passing day underscores the urgency of expanding Covid-19 vaccine access. The gulf between vaccine haves and have-nots has been denounced as “vaccine apartheid". Huge inequities in government resources to procure vaccines and skewed manufacturing capacity have deeply influenced which countries can get vaccines first, and who gets vaccines within countries.
The key problem driving disparities in governments’ access to vaccines—as well as the corruption, grey market for vaccines, and the use of bribes that allow some to jump the vaccine queue—is an acute shortage of supply. A proposal India and South Africa brought to the World Trade Organization (WTO) could be a game-changer in addressing that problem.
By the end of February, over 100 countries had received vaccines, but more than half of the total of 210 million doses had gone to two countries; 80% were concentrated in 10 countries. It’s been a year since COVID-19 was declared a pandemic, its varied impacts have been devastating, and vaccine access delays will affect how quickly we can recover.
The Philippines government has been so desperate for vaccines that it reversed a ban on Filipino health workers migrating abroad, allowing them to seek jobs in Germany and the UK in exchange for vaccines. Italy opened an investigation into complaints that intermediaries were offering to sell vaccines on the grey market. Vaccine corruption scandals, with powerful politicians jumping the queue, have made headlines in South America, Spain, Lebanon and other parts of the world. Anger over the rich and powerful skipping the vaccine line is palpable.
How fast a country can move beyond rationing to broader vaccine coverage depends on a government’s access to vaccine supplies. The US, for example, has announced that it aims for all adults in the country to have access to a vaccine by May.
Europe has been hit by vaccine supply delays, causing a furore. In response, the European Commission restricted vaccine exports from EU member states, deepening the global crisis.
For five months we’ve watched a debate unfold behind closed doors about the proposal by India and South Africa. When it was first introduced, the World Health Organization (WHO) had reported over 1 million COVID-19 deaths worldwide. Over 100 governments now back India and South Africa. But a handful of mostly high-income countries—including the US, the European Union (represented by the European Commission), the United Kingdom, Canada, Australia, Switzerland, Japan, and Brazil—have blocked the proposal. In the five months that these governments have stonewalled at the WTO, another 1.5 million people have succumbed to COVID-19.
The proposal would allow WTO members to temporarily waive the application of some rules that are part of a global intellectual property treaty, called the TRIPS Agreement, until widespread vaccination is in place globally. Global intellectual property rules are complex and impede the ability of governments to swiftly respond to the magnitude of the crisis at hand. A temporary waiver could help low- and middle-income governments to fulfil their human rights obligations to protect people’s lives and health. It would give governments leeway to pursue the fastest possible route to scale-up vaccine manufacturing by tapping unused or under-used factories anywhere in the world.
Wealthy governments’ continued opposition to the TRIPS waiver is unconscionable. These governments have the money and infrastructural resources to procure or manufacture vaccines, which a vast majority of low-and-middle income governments don’t. Their opposition is not just duplicitous but dangerous. They are blocking poorer governments from being able to use all possible measures at the national level for an effective COVID-19 health response.
It also ignores their basic human rights obligations for international cooperation and assistance, health and sharing the benefits of scientific progress. While governments have an obligation to protect their own populations, they have a co-existing obligation not to act in ways that impede other governments from meeting their responsibilities. All governments have a duty to engage in international cooperation and assistance to ensure universal equitable access to vaccines.
While blocking one of the most effective measures to help others, many of those same countries are pledging charitable donations—of money or surplus vaccine doses from what they’ve already pre-booked. The European Commission, Canada, Australia, Switzerland, Japan, and several other governments point to their donations to COVAX, a global vaccine procurement facility, using that as an excuse to deflect attention from their unfair stance at the WTO. The EU promised to double its donations to COVAX, totalling €1 billion. The US reversed its COVAX snub, pledging up to $ 4 billion over three years.
More money to COVAX is good news. It will subsidise the vaccine bills for 92 low-income governments. But charitable donations are not a sufficient response and fall short of the collective cooperation response needed to maximise vaccine production for all.
The COVAX facility will help increase the odds of equitable vaccine access but is not a substitute for what the TRIPS waiver can enable. COVAX aims to vaccinate only 20% of every participating country’s population. That’s far from what is needed to reach herd immunity in countries that rely heavily on it as their source of vaccines. Supply challenges and delays hamstring COVAX too. The facility has estimated in early February that it can procure and distribute enough vaccines for 3.3% of all countries’ populations—to cover health workers by mid-2021.
Sadly, money doesn’t magically produce vaccines or ease the tangle of complicated global rules surrounding vaccine manufacturing, exports and imports. South Africa said recently at the WTO General Council meeting, powerfully, “The problem with philanthropy is that it cannot buy equality…. If there are no vaccines to buy, money is irrelevant.” A purely philanthropic approach doesn’t solve the problem. As South Africa continued: “the model of donation and philanthropic expediency cannot solve the fundamental disconnect between the monopolistic model it underwrites and the very real desire of developing and least developed countries to produce for themselves.”
Where throwing money at the vaccine supply problem and the maze of trade rules that delay vaccine delivery will not speed up vaccine manufacturing, governments acting on their rights obligations can. Governments have before them a clear pathway, based on international cooperation and prioritising everyone’s rights—and their right to health in particular, which could lead to a fair post-pandemic world.
To go down that path we need courageous leadership that suspends rules that are barriers to expanding life-saving vaccine access. Calling on world leaders to unleash the power of manufacturing and vaccinate faster, Dr. Tedros Adhanom Ghebreyesus, the director-general of the World Health Organization, supported the waiver, asking poignantly: “If not now, when?”