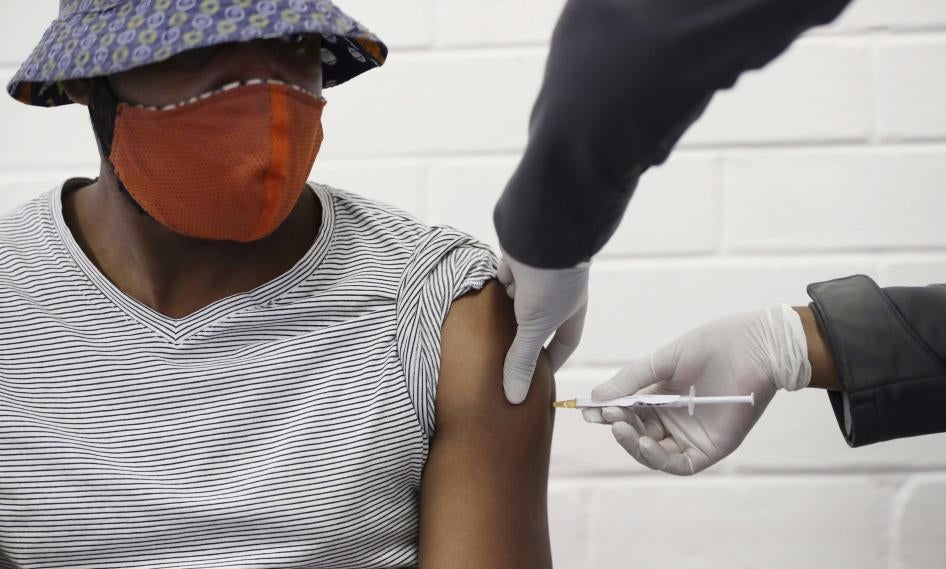
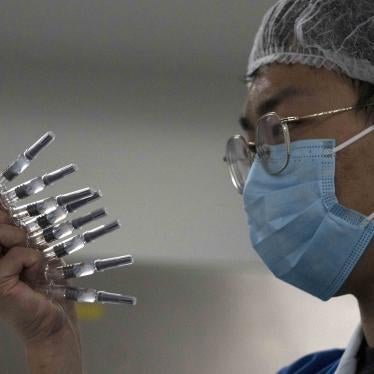
The warnings about vaccine nationalism started early.
As governments poured massive amounts of public money into the race to develop Covid-19 vaccines, experts from around the world warned that, with limited supplies, vaccines would not become a global public good if rich countries were able to monopolize or dominate the available doses only for themselves.
World leaders, human rights and public health campaigners, Covid-19 survivors, and loved ones of those who died came together to call for a people’s vaccine. “Our world will only be safer once everyone can benefit from the science and access a vaccine,” they wrote last May in an open letter.
As people around the world waited anxiously for a safe and effective vaccine to be developed and approved, it became clear that some would be waiting much longer than others.
News in late 2020 that several vaccine candidates in the pipeline were found to be safe and effective brought hope.
But in mid-January, Director-General Tedros Adhanom Ghebreyesus of the World Health Organization (WHO) warned that the world was “on the brink of a catastrophic moral failure – and the price of this failure will be paid with lives and livelihoods in the world’s poorest countries.” The “me-first approach” rich countries were taking would “leave the world’s poorest and most vulnerable people at risk,” he said, and “It’s not right that younger, healthier adults in rich countries are vaccinated before health workers and older people in poorer countries.”
By the end of February, vaccine doses had reached over 100 countries, but more than half of all the doses had gone to just two countries, and 80 percent had gone to 10 countries.
In short, the world is in exactly the situation that Human Rights Watch and many others had been warning against. Vaccines that are in short supply are going to the highest bidders, undermining the WHO’s broad guidelines for equitable allocation, which advise prioritizing health workers, older people, and people with underlying health conditions. Former Liberian president Ellen Johnson Sirleaf expressed frustration, arguing forcefully for treating “vaccines as a global good to be able to save humanity…. They cannot treat it as apartheid. They cannot say because you’re poor, you will not be vaccinated, only the rich will be.”
The devastating impact of inequitable distribution—in which large portions of the world’s population, including the most at-risk populations within individual countries, do not have timely access to a safe and effective vaccine—should not be underestimated. Universal and equitable vaccine access is needed to save lives, prevent people from experiencing severe illness and potential long-term negative health impacts, ensure that children return to school, and enable economies to rebuild and families to make ends meet.
Like other infectious diseases, Covid-19 can spread rapidly across borders. No one country’s people or economy can be fully protected from a deadly infectious disease until all countries are protected. Economists projected that vaccine nationalism could cost the global economy more than US$9 trillion because uneven vaccine access will prolong the pandemic and delay global economic recovery.
Many countries that lack the power to negotiate bilateral deals with pharmaceutical companies are relying on the COVAX Facility, a vaccine procurement mechanism led by the WHO and two public-private partnerships: Gavi, the Vaccine Alliance and the Coalition for Epidemic Preparedness Innovations. COVAX aims to provide participating economies with enough doses to cover at least 20 percent of their populations in 2021.
COVAX has been offered up as an alternative to vaccine nationalism and it is essential for governments and international entities to cooperate. But COVAX does not solve the vaccine scarcity that led rich governments to prebook vaccines in the first place. And COVAX, as it is envisioned now, will not deliver the vaccination coverage needed on a global scale to halt the pandemic.
COVAX has announced plans to roll out doses covering about three percent of the populations of participating economies in the first half of 2021, with the goal of providing vaccines for 20 percent of participants’ populations by year’s end. Unfortunately, this would still leave the world nowhere near the vaccination coverage needed to reach herd immunity. Meanwhile, middle-income countries have begun negotiations on their own, too. In Uganda, for example, people are questioning reports that their government paid 20 percent more than South Africa’s, and triple what the European Union paid, for AstraZeneca’s vaccines.
The world desperately needs to scale up vaccine manufacturing to achieve universal and equitable vaccine access. Governments and pharmaceutical industry leaders should come together to create a smart mix of regulatory and voluntary mechanisms to make this happen.
Governments should use their regulatory and spending powers to create incentives and require companies they fund to share the underlying intellectual property through technology transfers and open, nonexclusive licensing. This will enable qualified manufacturers anywhere in the world to produce as much vaccine as possible, as safely and quickly as possible, and at affordable prices. All governments, especially those funding vaccines, should join, and urge companies to join, the WHO’s Covid-19 Technology Access Pool to enable the kind of sharing that could lead to a global, cooperative approach.
Human Rights Watch has joined many other groups urging support for a proposal before the World Trade Organization that would waive some intellectual property rights for medical products until “widespread vaccination is in place globally.” The proposal—put forward in October by India and South Africa—would enable technology transfer and the sharing of intellectual property to ensure that vaccines and other medical products are widely available and affordable for all. Over 100 governments have supported this proposal. But a handful of high-income governments, including the United States, the United Kingdom, the EU, and others, have blocked it.
Recent export controls on vaccines announced by the EU, and the possibility that we will need repeat vaccine boosters beyond an initial vaccine course to provide lasting protection make it even more urgent to shore up supply.
Companies, too, have a role to play. They should share their intellectual property and set prices that maximize affordability for all users and minimize government debt. Companies should build public confidence in their efforts by publishing contracts and reporting transparently on their steps to prevent and minimize human rights risks.
It’s not too late for governments and companies to take all possible measures to provide universal and equitable access to safe and effective vaccines.
Our best hope is an approach grounded in cooperation, not competition.