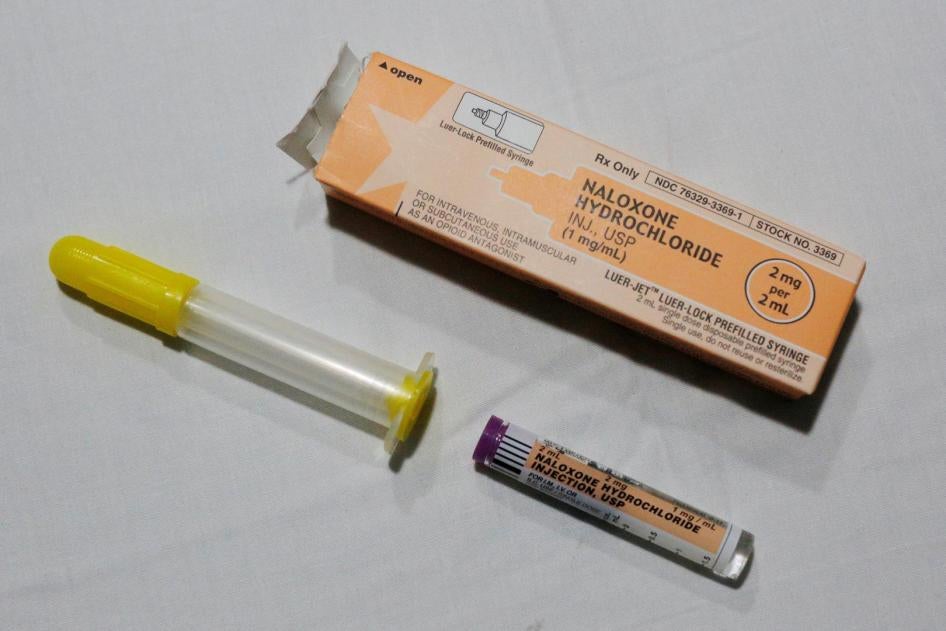
Most of these deaths involve opioids such as the powerful synthetic drug fentanyl, heroin and prescription painkillers. Naloxone reverses opioid overdose, but it must be given quickly. It is easy to use and has been successfully administered for decades by lay people, saving tens of thousands of lives. But its status as a prescription medication limits its availability. Making this antidote available over the counter could be a game-changer in reducing the terrible toll of preventable opioid overdose deaths.
The commission’s report notes the importance of increased naloxone access, but focuses its recommendations on expanding access among medical first responders. While this is important, it ignores the fact that the first people on the scene of an overdose are usually not emergency workers but friends, family members, and associates of people who use drugs. In this context, these people are the true “first responders.”
Naloxone access has increased significantly in the last several years, as nearly all states now permit naloxone to be prescribed to people who aren’t themselves at risk of overdose but who may be able to help someone who is. Similarly, most states allow for “standing orders” that allow for wider distribution of naloxone through pharmacies and, in some states, other venues. While these initiatives are important, they leave behind many of the most vulnerable Americans — those who do not regularly see a health care provider or who do not have insurance.
Human Rights Watch has documented in the U.S. and around the globe, many people who inject drugs are wary of interaction with the healthcare system because of stigma or poor treatment. Karen, whose real name has been withheld to protect her privacy, is a case in point. This 23-year-old former heroin user from Wilmington, N.C., told Human Rights Watch that talking to a pharmacist about what they need for their heroin habit is a difficult thing for lots of people. She says there is lots of fear and shame. Also, studies show that due to fears of arrest and prosecution, many people at the scene of an overdose are reluctant to call 911.
Why not just put naloxone in that person’s pocket? Time is of the essence with overdoses, and empowering people who witness an overdose to reverse it can prevent a delay that can result in death or irreparable brain damage.
Some enterprising states and cities have found ways to get naloxone into the hands of laypeople, and the results are exactly as expected. A recent study in Massachusetts found that cities that have naloxone distribution programs have lower overdose death rates than those that don’t. Similarly, the North Carolina Harm Reduction Coalition has given out 52,000 naloxone kits since 2013 through their statewide grass roots network that includes syringe exchange and naloxone distribution, with more than 8,700 overdose reversals reported. Because naloxone is a prescription medication, however, these results are difficult to replicate in other states, where distribution by community groups is often not permitted by law.
There is no reason why at least some formulations of naloxone could not be made available over the counter, which would make it far easier for these types of low threshold programs to provide naloxone to those at highest risk of overdose. Designated an “essential medicine” by the World Health Organization, naloxone is not a controlled substance and has no potential for abuse. It meets the criteria for over-the-counter status established by the Food and Drug Administration, and two of the mostpopular naloxone products were specifically designed for use by lay people.
The FDA is taking a number of steps, including preparing a model label and initiating the necessary trials to ensure that naloxone can be successfully used without prior training, in anticipation of a manufacturer requesting permission to sell naloxone over the counter. To date, however, none of the companies producing naloxone has done that.
The opioid commission missed a perfect opportunity to endorse community-based naloxone distribution, a proven, evidence-based, and common-sense strategy to reducing overdose deaths. A recommendation for the FDA to intensify its efforts to make naloxone available without a prescription would have increased the pressure on naloxone manufacturers to file the necessary applications — or, failing that, for the FDA to take that step on its own. In a public health emergency, every day we wait means more preventable deaths. The time to act is now.
Megan McLemore is a senior health researcher at Human Rights Watch. Corey Davis is a senior attorney at the National Health Law Program.