(Nairobi) – The Covid-19 pandemic has exposed gaps in health services that require urgent attention in many African countries, Human Rights Watch said today.
African governments should urgently address healthcare deficiencies to meet the demands of the Covid-19 pandemic and ongoing healthcare needs of their populations. They should act to ensure everyone’s right to health is in line with international human rights law, including the African Charter on Human and Peoples’ Rights.
“The current global health crisis from the spread of the novel coronavirus has brought to the fore the need for African Union (AU) member states to carefully analyze the current state of their healthcare infrastructure and make meaningful investments to improve access to quality health care,” said Carine Kaneza Nantulya, Africa advocacy director at Human Rights Watch.
In April and May 2020, Human Rights Watch interviewed African health experts, including pathologists, epidemiologists, and public health officials. They said that inadequacies in resources are due to insufficient government investment in health, which in turn affects the ability of health workers to fulfill their duties, especially during the pandemic.
The health experts and representatives of human rights organizations interviewed said that a chronic lack of investment in healthcare infrastructure and equipment has made it harder for African nations to retain skilled healthcare workers, provide essential medicines, and reduce the mortality rates of perennial diseases like malaria.
According to the World Health Organization (WHO) as of June 8, 187, 875 cases of Covid-19 had been reported across 54 African countries. The global health agency warned on May 7 that up to 190,000 people could die on the continent and up to 44 million could become infected, if the disease is not contained.
Lack of access to testing is hampering efforts to save lives, some experts told Human Rights Watch. While many African countries have responded swiftly by enacting measures to slow the spread of the pandemic, many also lack the capacity to test for Covid-19, isolate people with confirmed or suspected cases, trace contacts, and treat those with severe illness.
In 2001, African leaders signed the Abuja Declaration, voluntarily pledging to allocate a minimum of 15 percent of each country’s national budget to health. Nineteen years later, there have only been modest increases in the health budgets of a few African countries. In 2011, WHO reported that 27 countries had increased the proportion of total government expenditures allocated to health since 2001.
According to a subsequent report released in 2013, only three countries had attained the percentage pledged: Botswana (17 percent), Rwanda (20 percent), and Zambia (16 percent). In 2019, the Pan-African Parliament and the WHO Regional Office for Africa said that African governments should ensure the right to health for all and increase domestic resources for HIV prevention and treatment and overall health.
Norman Matara, a Zimbabwean doctor, told Human Rights Watch that African governments need to take the Abuja Declaration seriously. “When you look at the defense budget, they buy state-of-the-art military equipment, so this is not about poverty; it is about genuine political commitment,” he said. “Our health sector is poor…. This is not something that will change overnight. But if we continuously invest, we will see progressive, then full, realization of the right to health.”
Recent studies have highlighted deficiencies in health systems across the continent. A May survey report by Reuters found that there is less than 1 intensive care bed per 100,000 people across Africa, while an April report by the United Nations Economic Commission for Africa (UNECA) concluded that healthcare systems across the continent are under-resourced, with lower proportions of available hospital beds, intensive care units, and health professionals than other regions of the world.
Lack of consistent planning for healthcare infrastructure and inadequate funds allocation, compounded by budgetary cuts, have left public health sectors in some countries ill-prepared to deal with the novel coronavirus in Africa.
Solomon Dersso, chairperson of the African Commission on Human and Peoples’ Rights (ACHPR), the primary AU human rights entity tasked with promoting and protecting human rights on the continent, said the Covid-19 pandemic underscores the fact that health is a fundamental human right and that its realization and fulfillment is not just for the health of individuals but for the society as a whole: “Ultimately, the right to health is a policy choice,” he told Human Rights Watch. “Governments have the primary responsibility to be at the forefront of preventive and palliative measures.” He said African nations should pause and reflect during the current crisis.
In a March 24 statement, the ACHPR said that governments should provide health workers with the necessary protective equipment and establish treatment protocols to ensure that they are protected from exposure to infection. The commission also highlighted the importance of integrating human rights within the continental response to the pandemic in a May letter to the AU chairperson, President Cyril Ramaphosa of South Africa.
The right to health is a fundamental right under international human rights law. It is also a critical component of the UN Sustainable Development Goals (SDGs) and is recognized in at least 115 constitutions across the world, including the 55 AU member states. A key goal of the AU’s Agenda 2063, the institution’s master plan for democratic governance and sustainable development, is to ensure that citizens are healthy and that adequate investment is made to expand access to quality health care.
Article 16 of the African Charter on Human and Peoples’ Rights guarantees the right of every individual to enjoy the best attainable state of physical and mental health. The charter says that AU member states should take the necessary measures to protect the health of their people and to ensure that medical services, goods, and facilities are available, accessible, and of good quality.
“Beyond the current pandemic, African governments should bring the right to health front and center in their policies and programs to improve people’s lives,” said Kaneza Nantulya. “They should engage African human rights institutions like the ACHPR as key partners to fulfill their obligations under the African Charter.”
Lack of Adequate Protective Equipment, Insufficient Wages, Low Morale
A doctor in Soweto, South Africa, who, along with some of the others interviewed, requested anonymity to speak freely, told Human Rights Watch that the government’s neglect of adequate protective equipment and other factors threaten nurses’ lives and affects their morale:
We are overstretched and are not sufficiently protected. Our wages are being reduced but I still must pay for my own personal protective equipment (PPE). If I die, I am gone. Many nurses and doctors have left the country at a time when nursing colleges have been closed, so medical staff end up not getting solid qualification. We get low wages and are unmotivated. We have not received the promised 5.5 percent increase of salary, instead they cut our pay by 1 percent since the Covid-19 pandemic. My salary has not improved for the last three to four years. I am tired, very tired.
A Tanzanian nurse said:
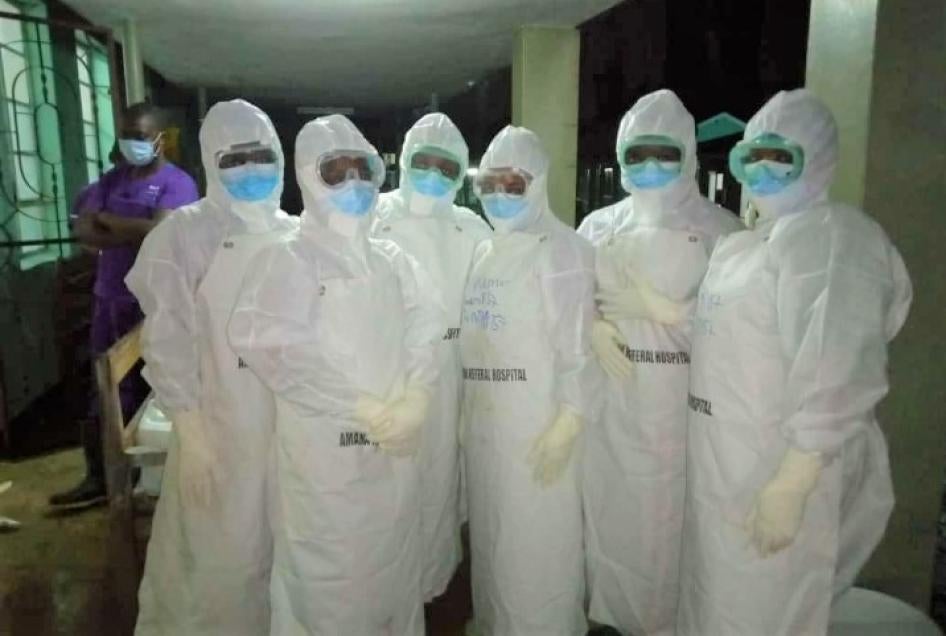
I have been working at Amana Regional Referral Hospital for 10 years. Here is what my normal day looks like: I do not have any PPE, but I commute in public transport. How am I supposed to protect myself and others? How am I supposed to protect my family? We are struggling …we hear that nurses abroad are well paid, so we consider that as the best option …people are demoralized.
Dr. Matara spoke about the Zimbabwean government’s longstanding neglect of health workers and the public health sector:
Doctors went on a strike for five months. They were paid for the first month, and then the government fired close to 400 doctors, although the sack was reversed after one month. I have been involved in more than 10 strikes in the last 9 years. What is peculiar about our most recent strike is that we were asking the government to provide us with basic equipment, gloves, PPE. We took the government to court and we won the court case. The government was compelled to provide PPE to health workers. Our senior government officials keep flying to China, Singapore, and South Africa to get treatment. Covid-19 had to come for the government to realize that it was important to rehabilitate hospital facilities – how ironic.
Lack of Long-Term Investment in Health Facilities, Local Expertise
Speaking about the lack of basic equipment, Emmanuel Othieno, a senior pathologist at Uganda’s Soroti Hospital, said:
Our biggest challenge is the lack of diagnostic laboratories. Patients and doctors are still consulting private labs. Sometimes samples are taken outside of the country for diagnosis, without proper records. We do not have a nationwide data management system, not to mention diagnostics. We have lots of referrals to India. When testing results are delayed, the fear of rising death tolls becomes real. We should avoid patients always having to travel abroad for testing and treatment.
A Burundian medical student in New Delhi, India said:
We want our governments to do the simplest things: provide diagnostic labs for our medical schools. How can we provide quality service when some countries do not have a single research facility within entire medical schools? I honestly do not intend to work in an African country. It is a waste of time. I have studied too hard, too long for this.
Dr. Awada Mohamed, director of the Centre Hospitalier Universitaire Ignace Deen in Conakry, Guinea said: “A major challenge is that we do not have enough nursing staff and care givers. The government does a lot, but we need personnel.”
Professor Oyewale Tomori of Nigeria, senior health expert based in Nigeria and a former WHO official, spoke about the importance of an “enabling environment” to build health system capacity:
The Lassa flu was discovered 50 years ago in Nigeria … we are a continent that fails to learn lessons. Every time we have a Lassa outbreak, we always approach it as a new outbreak. In 1989, I taught a young United States-based medical student here in Nigeria. But when the flu broke out again in 2019, my former student was invited to the country as an adviser to a panel on which I served. That is because he evolved in an environment that appreciated his skills and enabled him to grow his expertise. It is not enough to build local capacity; you must create an enabling environment for the capacity to function effectively. Also, Africa must learn how to upgrade and appreciate its medical expertise.
Right to Health and Covid-19, and Previous Disease Outbreaks
The experts said that many African governments’ responses to previous outbreaks of diseases such as measles, HIV, and malaria suggest that governments will not recognize the need to prioritize investment in the health sector after the Covid-19 pandemic.
Silas Majambere, a Burundian malaria expert, said:
I am unsure about governments’ abilities to learn from this crisis. Despite having hundreds of thousands of Africans dying of malaria each year, African governments have failed to invest in research for its treatment, or in the manufacturing of preventive bed nets locally.
Lassa fever is a severe viral hemorrhagic fever (VHF), like Ebola, that was declared an “active outbreak” by the Nigeria Centre for Disease Control (NCDC) in February 2020. Edobor Emiogun, a Nigerian independent health consultant, said:
The Lassa flu kills more than Covid-19 but no one does anything, because it is seen as “the poor man’s disease.” Covid-19 in a way has now equalized people, but I am not sure whether our leaders will learn anything from it.
On possible lessons to be drawn from the Ebola epidemic in Guinea, a Senegalese expert, Professor Fay Sylvain, said:
Not much was learned from our Ebola experience. We now have in some of our neighboring West African countries many Covid-19 patients lying in the corridors. Yes, we have the expertise, the know-how, but beyond this, have we increased our testing capacity? Where are our laboratories? How many hospitals have we built since the recent Ebola outbreak in 2013?
An ACHPR commissioner, Jamesina King, said:
We must go back to the drawing board. Allocating more funds … to health care is a must for African States. After Covid-19 should be the opportunity to address emergency health care, healthcare infrastructure, and a comprehensive health insurance scheme in Africa so that no one dies because they are too far from a health facility or they cannot afford expensive private hospitals. States should make healthcare systems in Africa sound and efficient so that the privileged do not always travel abroad to seek medical care.
Dr. Djoudalbaye Benjamin, Africa Center for Disease Control’s head of policy and health diplomacy, cautioned against a one-size-fits-all approach:
We must realize that deficiencies are multisectoral and consider that we have 55 countries; 15 percent from government GDP is not enough to build resilient systems, and it does not consider the economic discrepancies between countries. If you take South Africa, Morocco, and Burkina Faso, you immediately see that the impact will be different. We must go beyond the 15 percent, re-evaluate our methods of calculation of the allocation. This is important work that must be undertaken.
Speaking about governments’ lack of investment in the health sector, a Ugandan senior public health expert said:
The minister of health once told me that the public health expenditure had increased, but when I insisted and asked to see their budgets and figures, they realized that they had been decreasing their health budget per capita. At that time, they were spending US$10 per capita while WHO standards were $40 per capita. They had not known for some time because they were not tracking their health budgets. We must take advantage of Covid-19 to make the case to expand and track our health investments.
On the importance of building an efficient and equitable health system, Professor Salim S. Abdool Karim, a South African clinical infectious diseases epidemiologist, said:
On the issue of the Covid-19, we must remember that human beings will always be faced with a virus which we have not found out yet as we do not have an endless natural immunity. Let us be ready. If I could turn back the clock, we could have created a much more equitable medical system. Medical care is critical, you need a good and solid medical system, for any threat – it’s not just about equity but also about efficiency, power, correctness – a medical system that provides health promotion, both preventive and curative.
A UN secretary-general’s policy brief published in May on the impact of Covid-19 in Africa says that Mauritius has the second-highest level of preparedness for Covid-19 on the continent. Speaking about Mauritius’ perceived success in addressing the pandemic, Dr. Catherine Gaud, a Mauritian immunologist and a government adviser on Covid-19, said:
Mauritius has a lot to offer in terms of best practices. As of May 21, 2020, we have not had new cases for 23 days and we are conducting 3,000 screenings per day. Besides our natural advantage of being an island, because it is easier to control people’s movement in and out of the island, we have had universal health coverage, a strong laboratory system where we even conduct molecular biology, and a strong political will. Like in some African countries, we have adopted a multisectoral approach, and meet every single day with representatives from finance, military, foreign affairs, commerce, and, quite interestingly, the attorney general.
Legal and Policy Framework
Key relevant standards relating to the right to health include general comments by UN human rights treaty bodies, institutions monitoring the implementation of treaties. These include General Comments No. 14 (2000) and No. 22 (2016) of the Committee on Economic, Social, and Cultural Rights, and General Comment No. 15 (2015) of the Committee on the Rights of the Child.
In 2008, the ACHPR adopted Resolution 141 on Access to Health and Needed Medicines in Africa in 2008. The Resolution, which says that governments should take various measures and precautions to guarantee access to essential medicines and treatments for citizens, reaffirmed Article 16 of the African Charter.
The AU specifically addresses women’s right to health in the Protocol to the African Charter on Human and Peoples’ Rights of Women in Africa (“Maputo Protocol”) of 2003. Article 14 of the Maputo Protocol provides comprehensive provisions about the right to health, including sexual and reproductive health.
The African Union has endorsed various policy and normative tools, including: the 2015 Addis Ababa Action Agenda on the Third High-Level Conference on Financing for Development; the Global Strategy for Women’s, Children’s and Adolescent Health 2016-2030; the Catalytic Framework to End AIDS, TB, and eliminate Malaria by 2030; the Continental Policy Framework For Sexual and Reproductive Health and Rights (SRHR) and its Maputo Plan of Action 2016-2030; the Pharmaceutical Manufacturing Plan for Africa; the African Regional Nutrition Strategy 2015 – 2025 and the AU Decade on Traditional Medicines.
The Africa Health Strategy (AHS) 2016-2030 advocates stronger collaboration among various stakeholders, including government, civil society, and the private sector to better leverage knowledge and expertise and mobilize resources.