When 14-year-old Hassina had still not given birth after more than two days of labor, her family started to worry. She was bleeding and had passed out more than once from exhaustion and pain. The nearest hospital was miles away. Ambulances had not been seen for years in the war-torn Nuba Mountains – the area of Sudan she called home – and nobody in her village owned a car.
Fearing for the mother-to-be and her baby’s life, the family opted for the only means of transport available: a motorcycle. Wedged between the driver and a relative seated behind her to hold her upright, Hassina was taken on a two-hour-drive along bumpy dirt roads to a larger village. There, the men and Hassina waited for a car. By the time Hassina reached the hospital, the baby had died.
Hassina, now 19, lives in rebel-held Southern Kordofan, a region in Sudan that, following the separation of South Sudan in 2011, has become the site of conflict between forces of the Sudanese government and the rebel Sudan People’s Liberation Movement-North (SPLM/A-North). Six years of on-and-off fighting and bombings by Sudanese government planes have led to hunger, widespread displacement, and destruction of schools, health clinics, and homes. The situation has also had a devastating effect on women’s and girls’ health.
A new Human Rights Watch report, “No Control, No Choice,” shows how both warring parties have obstructed humanitarian aid from reaching the region, leaving women living in rebel-held areas with virtually no access to contraceptives, trained health workers, or well-equipped clinics that could provide preventive or emergency health care for women of childbearing age.
As a result, young women like Hassina have little control over the number of children they bear or the spacing of their pregnancies. Instead they rely on local birth attendants, who often lack formal training or, like Hassina’s midwife, have lost their equipment in government attacks. As many local clinics do not even have stethoscopes or kits to measure blood pressure, the young mothers-to-be risk dying in childbirth or losing their newborns.
At 19, Hassina had already lost three.
Like many girls in the region, Hassina got married while still a child. With no end to the conflict in sight, her family had found it increasingly hard to feed her and her siblings and saw marriage as a way out. Although marrying that young can cause harm to a girl in many ways, including early childbearing, nobody talked to Hassina about sex or family planning. The lean, soft-spoken young woman had never seen a condom or heard about contraception.
Wrapped in a pink, flower-embroidered cloth called tobe, her voice a mere whisper, Hassina tells her story– a story of pain, loss, and lack of control over her body and life.
When pregnant with her first child, the only prenatal care she received consisted of a local midwife touching her belly and telling her she would be fine. With only two hospitals left in the region to serve hundreds of thousands of people, the nearest full prenatal care is at least one full day’s walk away from Hassina’s village, Hadara. At the time, Hassina did not make the long journey for regular check-ups. Hence, she only learned that her cervix was too narrow to give birth vaginally after the emergency caesarean section that saved her life.
Without access to contraception or knowledge about family planning, she soon became pregnant again.
Knowing she might risk losing another baby during childbirth, Hassina did what many Nuba women with a history of birth complications do when close to term. When she was around seven months pregnant, she embarked on the long walk to the hospital, where she knew professional help would be available to deliver the child. For weeks, she camped in the shade of trees near the hospital, waiting for the contractions to start. Again, she had to have a caesarean, but this time the baby was born alive and healthy. Six months later, however, her little boy fell sick and died.
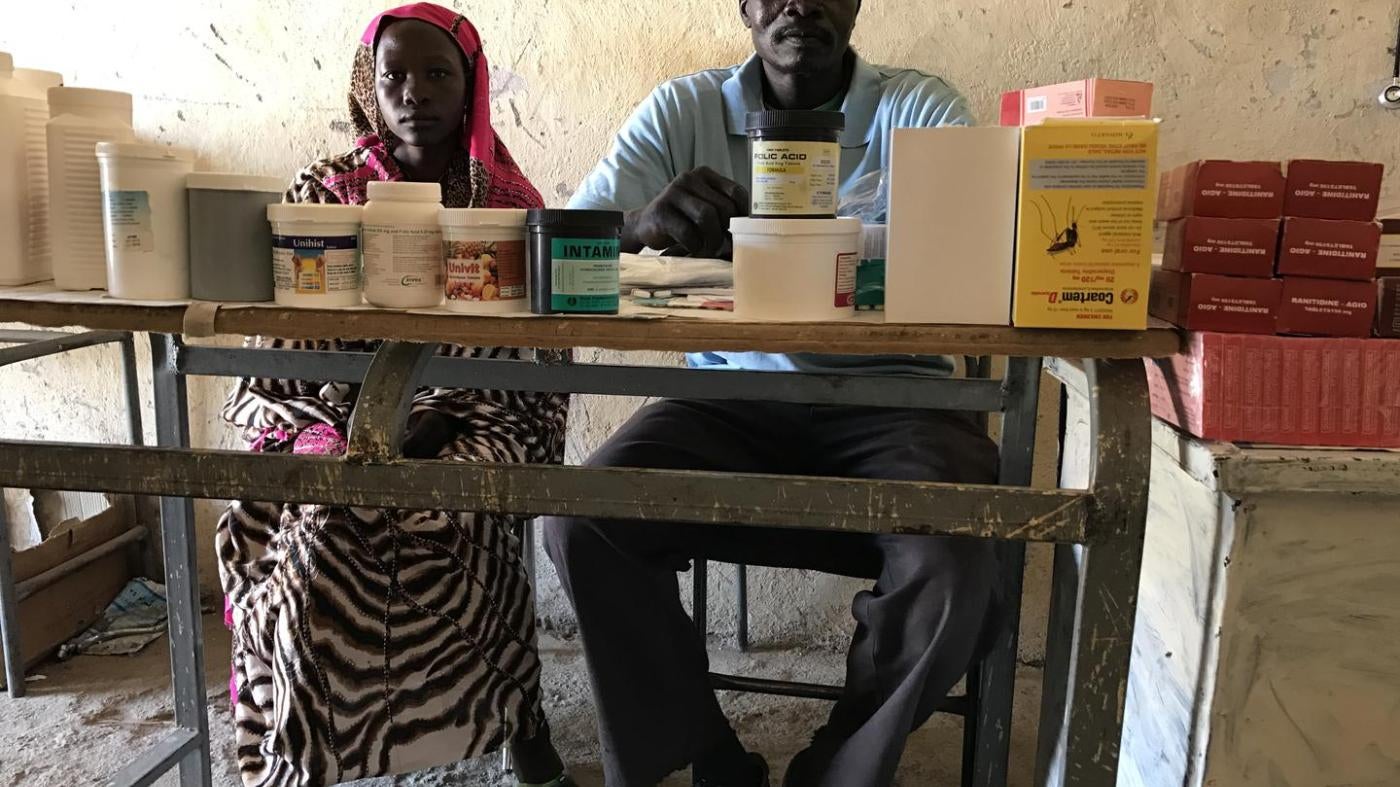
Many children in the region, health workers say, succumb to preventable childhood diseases before they learn to walk. Despite its bustling marketplace, Hadara, where all kinds of smuggled goods from cigarettes to tomato paste are traded, was already poor before the war began. Today, food is in short supply, and so are medicines. The village’s poorly equipped clinic has a patchy stock of antibiotics, deworming medication, and anti-malaria pills, which were dropped off by aid organizations that defy the ban on operating in the region. But vaccination campaigns for newborns have never reached the area. Even United Nations attempts have been stymied by the parties to the conflict.
Devastated, Hassina was well advanced in her third pregnancy, when, in 2015, Sudanese airplanes attacked, dropping bombs on Hadara. Then Sudanese ground troops moved in, torching most of the village, and forcing its inhabitants, including Hassina, to flee.
For weeks, Hassina and her family hid in a dried-up riverbed, while planes bombed the area and no cars were available to get to the hospital. She was still holed up in the riverbed when her labor began. After days of contractions and excruciating pain, the baby’s body cleared the birth canal. Its head, however, got stuck.
Her fingers fiddling uneasily with the seams of the pink tobe wrapped around her head, Hassina casts her eyes to the ground, recalling those painful hours during which her family searched for transport to get her to the hospital and have the head taken out.
Not once does she raise her voice in anger. Yet, if the Sudanese government and SPLM/A-North allowed humanitarian aid to the area, she and other Nuba women would have a much better chance of protecting their own health and that of their children – and Hassina might after all be able to have a baby that is born alive and survives.