“When I was 13… I got pregnant from my older brother… He raped me starting when I was 11,” a girl from Guatemala told one of us in 2015. She was one of the 2 million girls under 15 worldwide who give birth each year, often due to sexual violence.
The Covid-19 pandemic is putting girls like her at even greater risk. While lockdowns reduce the spread of Covid-19, they also drive a global spike in reported violence in the home, and leaving some women and girls isolated with abusers, leading to increased unwanted pregnancies.
The pandemic is putting enormous pressure on health systems around the world as governments work to contain the virus and treat sick people. But governments also need to sustain other essential services, which according to the World Health Organization include sexual and reproductive health services.
Overloaded hospitals, travel bans, lockdowns and border closures are making access to those services increasingly difficult. Poor and marginalized women and girls, including those with disabilities, especially risk losing access to needed services. And some governments’ responses are making matters worse by discriminating against women and girls who need them.
The pandemic is exposing and exacerbating existing inequalities. More than 5 million families in Africa, Asia, Latin America and the Caribbean already spent more than 40 percent of their annual non-food household expenditures on maternal health services before the pandemic. With poor families hardest hit by the pandemic’s economic consequences, they are likely to find it even harder to get quality maternal health care.
Governments need to make sure that people can get these services, regardless of ability to pay, and that pregnant women not only get pre-natal and birth care and have the right to make decisions about their labor and delivery plan.
But they also need to protect everyone’s choice about whether to become pregnant or continue a pregnancy. The International Planned Parenthood Federation reports that the pandemic has forced them to close thousands of family planning facilities—either due to government orders or social distancing needs— Colombia, El Salvador, Pakistan, Germany, Ghana, Malaysia, Sri Lanka, Sudan, Uganda, Zambia, and Zimbabwe have each had to close at least 100 such facilities.
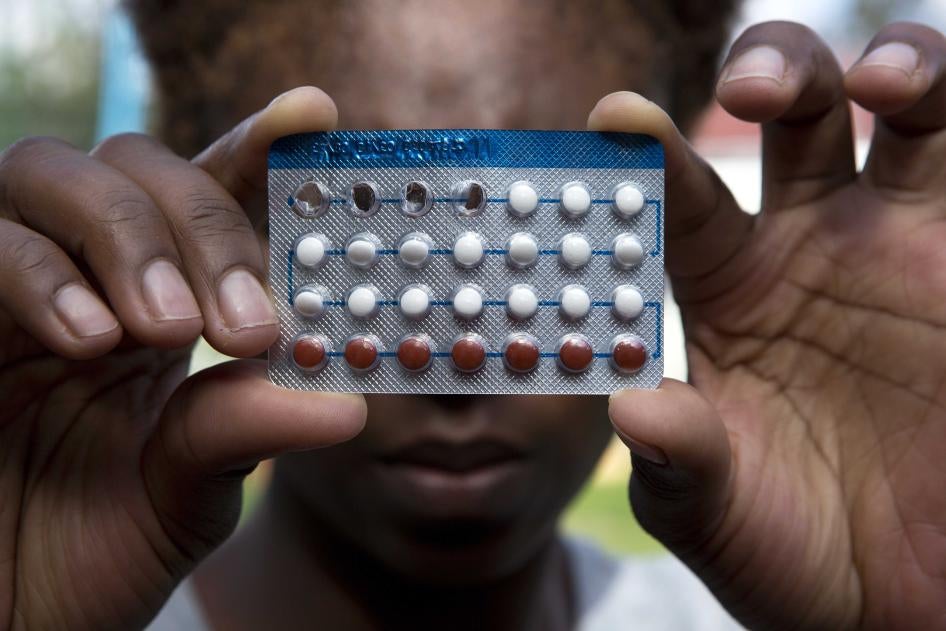
Directors for Marie Stopes, an organization that provides contraception and safe abortion services in many countries, in Uganda and Zimbabwe said they have waited in vain for supplies to arrive. “We’re expecting a huge shortage of contraceptives in African countries,” one said. In Venezuela, thousands of women who previously travelled to neighboring Colombia to obtain contraceptive supplies are now blocked by border closings. Manufacturers warn of a global condom shortage because manufacturers are locked down to halt the spread of the virus. The shortages of contraceptive supplies increase the risk of unplanned pregnancy, sexually transmitted infections, and the need for abortion.
Anti-choice politicians and organizations are capitalizing on the pandemic by urging governments to prohibit abortion care during the crisis. In the United States, 11 states have tried to limit access to abortion. Poland’s Parliament is considering regressive legislation to eliminate legal access to abortion in some cases and to criminalize sexuality education.
Abortion cannot be delayed, and denying access violates human rights.[[nid:339665 field_ne_alignment_limited=right]]
The right to non-discriminatory access to women’s health services is part of the right to health under international law and domestic law in most countries. Governments need to find ways to protect this right, even in the pandemic.
Denying these services will undermine women’s ability to recover from the pandemic. And increased pregnancies or unsafe abortions could increase pressure on already overburdened health systems.
The pandemic is reshaping our world, but it is also an opportunity to reshape reproductive health services. This might include expanded use of telemedicine, and making information available online. Expanding access to medical abortion at home, as England, Scotland and Wales have done, can help. In communities with limited access to technology, governments should ensure that health providers have the equipment and resources they need to safely reach patients.
Governments should monitor supply chains closely and seek solutions if contraceptive shortages arise, including redistributing available supplies across localities and even countries. They should ensure access to contraceptive information and services, including emergency contraception and abortion care.
Governments should put protecting sexual and reproductive rights up front in their response to Covid-19. These services are essential to women and girls—and their families– surviving and remaining healthy and are needed more than ever during the Covid-19 pandemic.
--
Anand Grover is the former United Nations Special Rapporteur on the right of everyone to the enjoyment of the highest attainable standard of physical and mental health and Ximena Casas is a women’s rights researcher at Human Rights Watch.