The Center for Disease Control (CDC) took an important step last week toward acknowledging the suffering of chronic pain patients in the United States who face unnecessary barriers to accessing opioid medications.
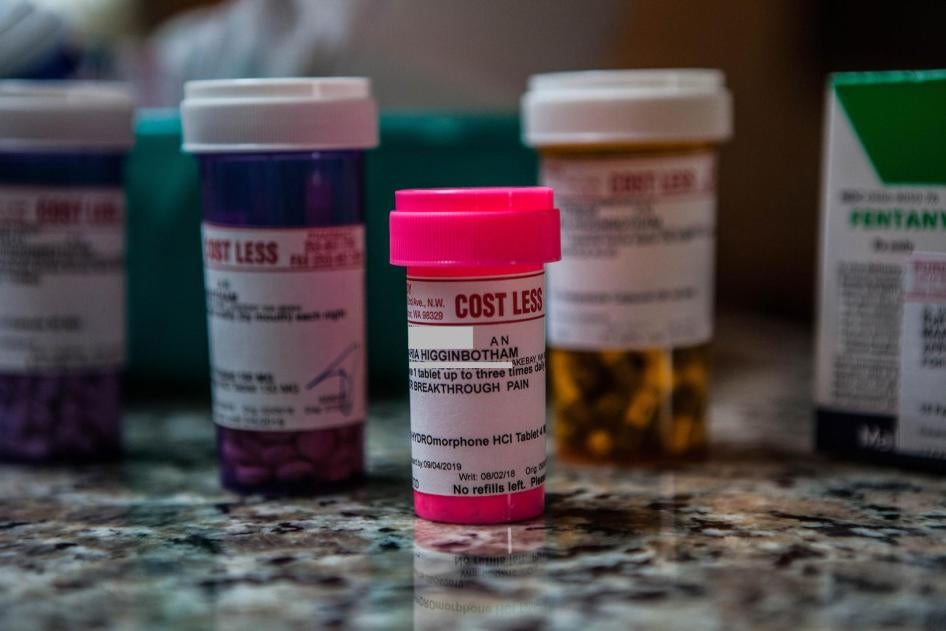
In 2016, the CDC issued a guideline to primary care doctors about how to prescribe opioids to new patients, including recommendations about the number of days and dosage amount, in an effort to ensure that physicians were safely prescribing the medication. Now, three authors of that guideline are acknowledging that it was widely misapplied by some medical providers, insurance companies, and pharmacies.
In December, Human Rights Watch documented how some physicians were involuntarily reducing opioid medication dosages for chronic pain patients because they feared liability or scrutiny from law enforcement, state medical boards, and insurance providers. Patients’ physical and mental health declined as a result. Some could no longer do simple things like walk their dog or go to the toilet unassisted, while others felt socially isolated, suicidal, or turned to alcohol or illicit drugs.
The CDC authors stated that their guideline was intended for patients new to opioids, not those who have been on them long-term and who benefit from them. They also noted that some patients may find weaning off opioids difficult.
“Some clinicians may find it easier to refer or dismiss patients from care. Clinicians might universally stop prescribing opioids, even in situations in which the benefits might outweigh their risks,” they wrote. Such actions “can adversely affect patient safety.”
The CDC is right to defend chronic pain patients against the unintended outcomes of its guideline. While reducing overprescribing is a laudable goal, it is important to acknowledge the collateral damage that has been done in pursuit of that effort.
But there’s still a long way to go. Many state laws, insurance companies, and pharmacies have policies that use the CDC guideline to enforce dose or day limits on opioid prescriptions. Oregon has proposed a policy that would deny opioids to a broad range of Medicaid patients with chronic pain – despite an expert letter condemning the policy as scientifically unsound. It will go to a final vote on May 16. There are concerns other states could follow suit.
The CDC took a big step in showing compassion for chronic pain patients. It’s time physicians, politicians, and policymakers across the US supported policies that did the same.