By Angela Chung
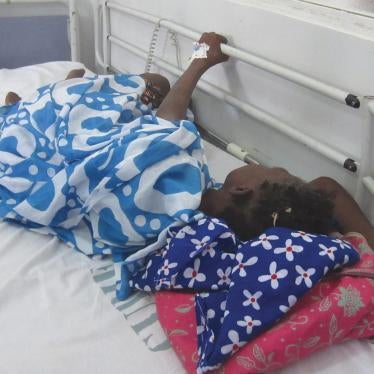
When Abdoulaye’s mother left his hospital bedside to pick up medicine from the pharmacy, I helped fan him. Temperatures in Senegal reach the 90s in November, and the air in the ward for children with advanced cancer hung hot and still. Flies buzzed, landing on the faces of patients who were too tired to swat them away.
Abdoulaye, age 4 ½, had a type of cancer that caused tumors to form on his bones, and is extremely painful.
For six months Abdoulaye received no morphine – a standard part of treatment in many parts of the world. When he arrived in the cancer ward, he received a few doses of the painkiller. Then Senegal ran short of morphine.
Because of the pain, Abdoulaye couldn’t speak. His feet and body were swollen from the cancer. He cried constantly, and would shriek whenever anyone lifted him.
My grandfather died of lung cancer, and it was horrible. But you don’t know how much worse it is when you don’t have morphine. You don’t even think about it until you don’t have that pill.
Morphine was still in short supply when Abdoulaye died a month later. His excruciating pain at the end could have been erased with the mere pennies it would cost for a dose of morphine.
Severe pain and other debilitating symptoms are common among patients with cancer, HIV, and other life-threatening diseases, particularly during the later stages. As I documented in my report, Abandoned in Agony, about 70,000 Senegalese each year need what is known as palliative care to control symptoms related to these diseases. Morphine is an essential and inexpensive medication for severe pain, but Senegal only imports about one kilogram of morphine each year – enough to treat about 200 cancer patients.
Why the shortfall? The country’s national pharmacy, where hospitals and health facilities get most drugs, does not import oral morphine, and restrictive regulations make it very difficult for patients to obtain the drug.Doctors were taught that morphine is a dangerous narcotic to be used only in extreme circumstances. Morphine is virtually never available outside of the capital, Dakar, where there are frequent shortages. Most Senegalese don’t know about morphine and many rural poor think no one can help their pain.
When I was assigned to work on palliative care issues at Human Rights Watch, I felt disappointed. I thought it wasn’t as important as my previous projects – genocide prosecution in Rwanda and combatting child pornography, prostitution and trafficking in the United States.
Now that I understand how vital pain relief is, I’m ashamed of my initial reaction. Before, I never realized how painful cancer is. In the developed world, painful diseases like cancer are censored because we have morphine. We treat pain relief like it is a luxury, as opposed to a basic response to suffering, a human right, an end to what is the equivalent of torture for many patients.
Ultimately, this project was the most difficult of any I had ever worked on. I had come across terrible stories from victims of genocide and sex trafficking, but, at the same time, there was hope. Those victims were rebuilding their lives.
With terminally ill patients in pain, there wasn’t that element of hope – their lives were probably not getting better without morphine. These patients were in pain, will continue to be in pain, and will ultimately die in pain. Some said they wished for death.
“Do you know where I can get the morphine?” Sohkna asked me. She had liver cancer and was in so much pain that she could only sit upright on her mattress, teeth clenched, clutching the edges, arms stick-straight like with rigor mortis. Or Oumar, who suffers from immense pain caused by prostate cancer and prepares for morphine shortages by rationing his pills. Some patients were certain that I could get them morphine. It was heartbreaking to tell them I couldn’t.
These patients literally have no voice – they’re in too much pain. Their relatives are too busy caring for them to push for change, and when it is over, too traumatized and financially strained. And the need for pain treatment is easy to overlook when war, famine, and natural disasters strike or the government focuses exclusively on curative care.
The thing is, we can fix this problem so easily. Want to ease people’s pain when they’re dying? All you need is morphine and minimal training for healthcare workers. With pain relief, these people and their families would have a chance at finding peace. If we could end a person’s excruciating pain with a pill, how could we ignore that?