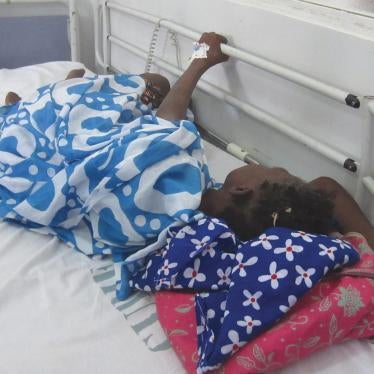
(Nairobi) - Kenyan children in acute and chronic pain suffer needlessly because of government policies that restrict access to inexpensive pain medicines, a lack of investment in palliative care services, and inadequately trained health workers, Human Rights Watch said in a report released today.
The 78-page report, "Needless Pain: Government Failure to Provide Palliative Care for Children in Kenya," found that most Kenyan children with diseases such as cancer or HIV/AIDS are unable to get palliative care or pain medicines. Kenya's few palliative care services provide counseling and support to families of chronically ill patients, as well as pain treatment, but lack programs for children. In addition, the majority of sick children are cared for at home, but there is little support for low-cost home-based palliative care. Health care workers lack training in pain treatment and palliative care, and even when strong pain medicines are available, they are often reluctant to give these medicines to children.
"Kenyan children with cancer or AIDS are living, and dying, in horrible agony," said Juliane Kippenberg, senior children's rights researcher at Human Rights Watch. "Pain medicines are cheap, safe, and effective, and the government should make sure that children who need them get them."
The Kenyan government has taken a step in the right direction by establishing a few hospital palliative care units in recent years, Human Rights Watch said. But much more needs to be done to stop sick children from suffering needlessly.
The mother of Gerard K., who lived in the Kibera slum in Nairobi and who died of complications associated with HIV/AIDS at age 5, described his experience: "[My son] had severe pain sometimes, especially some abdominal pains.... There were times that he would use those pain killers paracetamol and Brufen [ibuprofen] and the pain would ... just persist ... I could tell he was in a lot of pain because he was just stiffened and you could see he was really struggling ... he died in pain."
The World Health Organization considers oral morphine an essential medicine for treating chronic pain, as does Kenya's own drug policy. A daily dose can cost as little as a few cents. Yet, the Kenyan government does not purchase oral morphine for public health facilities as it does other essential medicines. As a result, oral morphine is available in just seven of the country's approximately 250 public hospitals. Although 250,000 people in Kenya are on antiretroviral treatment, all the morphine in the country could treat pain in only 1,500 terminal cancer or AIDS patients.
More than 1.5 million Kenyans are living with HIV/AIDS, including about 150,000 children, and 100,000 Kenyans die from AIDS each year. People with HIV can experience severe pain whether or not they receive antiretroviral drugs, and inexpensive pain medicines can improve adherence to HIV treatment, Human Rights Watch said.
International donors are also neglecting pain treatment, Human Rights Watch said. For example, the US President's Emergency Plan for AIDS Relief (PEPFAR) spent US$534 million in Kenya in 2009. PEPFAR finances palliative care services such as counseling at hundreds of health facilities, but few have morphine to treat severe pain.
Human Rights Watch called on the Kenyan government to make oral morphine available in all public hospitals, to ensure that health care workers are trained in palliative care, and to integrate children's palliative care into its health services, including home-based care.
"The Kenyan government, and donors, should be working to improve pain treatment for everyone," Kippenberg said. "And they should make sure that the youngest and most vulnerable sufferers, sick children, are not left out. They should not be suffering needlessly."
Testimony from providers, parents, and patients:
"Before I came [here], I couldn't eat or breathe well [because of the pain]. Now that I have been given medicine, I can eat and breathe. I couldn't sit down, but now I can. I had pain for more than a month. I told the doctor and nurses [at the Kijabe mission hospital] that I had pain. It took too long to get pain treatment in Kijabe. Here [Kenyatta National Hospital] I got it immediately and started feeling well again."
- Christine L., 18 years old, diagnosed with breast cancer when she was 17, Nairobi
"People have no problems with relieving pain in adults with morphine, but when it comes to children, there is always some reservation. Putting a child on morphine is always a big issue.... Morphine is underutilized."
- Doctor treating children with cancer, Nairobi
"The body and his wounds were very painful and eating was very difficult. He would refuse food and cry. Blood would come out of his mouth when we washed it.... He was in pain ... it would hurt him to bathe. He would cry because of wounds and peeling off of skin."
- Community health worker, Kisumu, describing the case of Douglas O., who died of HIV/AIDS at age 5. Douglas was prescribed anti-retroviral treatment but was in the care of his adolescent sister who did not always give his medicines regularly.
"We have no pethidine, no DF-118, and no morphine.... We have children here with advanced HIV; some are in severe pain. The pain management for children with advanced HIV is not enough."
- Nurse, Bondo District Hospital. Pethidine and DF-118 (dihydrocodeine) are pain medicines that are weaker than morphine.
"They ask you questions: ‘Why am I not going to school and my peers are going to school?' ‘Why am I not being allowed to play with my friends and my friends are playing out there?' ‘Why are you always taking me to the doctor and my friend so-and-so and neighbor are not always going to the doctor?'.... [Emotional support] is extremely important because they always ask, ‘Why is this happening to me?'
- Head doctor, Nairobi Hospice