It may be World AIDS Day, but the prospect of “an AIDS-free generation,” a goal articulated by US President Barack Obama, is uncertain. While new HIV infections in the United States have dropped nearly 20 percent in the past decade, African-Americans, men who have sex with men and transgender women are disproportionately afflicted by the disease.
President-elect Donald Trump has said little about the 1.2 million people living with HIV in the United States, leaving his policies on this health crisis a matter of speculation. That should be cause for alarm. An outbreak of HIV infections in Indiana while Vice President-elect Mike Pence was governor stands as a sober warning of how quickly an epidemic can emerge in the absence of strong and effective policies.
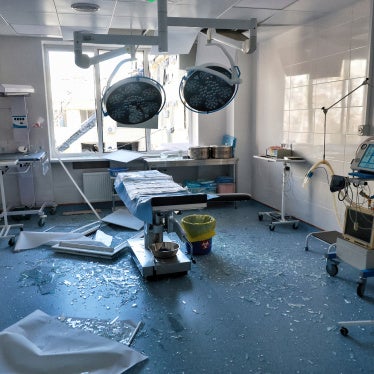
In December of 2014, the tiny town of Austin, Indiana, became the epicenter of one of the worst HIV outbreaks among injection drug users in decades.
Syringe exchange – a key tool in preventing the spread of HIV – was illegal under state law. Drug users in Austin routinely shared needles, a practice that carries a high risk of HIV transmission. Nearly 200 of Austin’s 4,200 residents – almost 5 percent of its population – became HIV-positive in one year, accounting for about one third of Indiana’s new HIV infections in in 2014. Of those infected with HIV, 84 percent also tested positive for hepatitis C.
When the outbreak was discovered, officials began a mad scramble to bring public health services to Scott County, where Austin is located. But the county was ill-equipped to deal with this emergency: It had only one primary care physician and no drug dependence treatment centers. Eventually, Pence allowed syringe exchange programs to begin operating on an emergency basis.
The CDC has since identified 220 other impoverished rural counties across the country that, like Scott County, are at high risk of HIV outbreaks among people who inject heroin or prescription pain killers. Some counties are responding by establishing syringe exchanges, distributing medicine that can reverse an overdose, expanding HIV education to reduce stigma, and encouraging HIV testing. But federal leadership is key to ensuring vital funding for syringe exchanges and other evidence-based approaches that prevent the spread of HIV. It’s also key in preventing the implementation of misguided and harmful approaches, like making syringe exchanges illegal. If the Trump-Pence administration shares the hope of seeing “an AIDS-free generation,” this is the path they should take.