Summary
Over the past two decades, Afghanistan has depended on international donor support to fund essential services like health care. But this donor support has been falling for years and will likely to continue do so—perhaps precipitously—following the announcement by United States President Joe Biden that the US will withdraw all US forces from Afghanistan by September 11, 2021. This decline in funding has already had a harmful—and life-threatening—impact on the lives of many Afghan women and girls, as it affects access to, and quality of, health care.
In the years after the US-led military invasion and the defeat of the Taliban government in late 2001, the Afghan government and international donors gave priority to developing an effective health system, including extending access to basic health care to all parts of the country. The effort led to important achievements, including significant declines in maternal mortality, and increases in provision of prenatal care, use of modern contraception, and attended births.
But even with two decades of effort and the expenditure of hundreds of millions of dollars, delivery of health services for women remains far below international standards, and the progress that has been achieved is being eroded in important ways.
Currently, women and girls struggle to access even the most basic information about health and family planning. There is an unmet need for modern forms of contraception; prenatal and postnatal care is often unavailable; specialty care, such as modern cancer and fertility treatment, is largely nonexistent; routine preventative care such as pap smears and mammograms are almost unheard of; and a large proportion of births are still unattended by a professional.
Health facilities often lack sufficient staffing and essential supplies and equipment. Afghanistan has 4.6 medical doctors, nurses, and midwives per 10,000 people, far below the threshold for critical shortage of 23 healthcare professionals per 10,000 people as defined by the World Health Organization. Women often struggle to access care due to costs, including for transportation to a health facility, and for medications and supplies for which patients are obliged to pay.
When they can obtain care, it is often of poor quality. Distance remains a problem for a significant proportion of the population; almost 10 percent of people cannot reach a health facility within 2 hours and 43 percent must travel more than half an hour. Lack of access to adequate care drives Afghans to spend US$285 million a year on medical tourism, mostly to Pakistan and India, draining funds from the health sector. Progress on some key indicators, such as accessing prenatal care and skilled birth attendance, is now stagnating, or even reversing. Corruption at all levels threatens the delivery of health services and demands for bribes drive people away from seeking care.
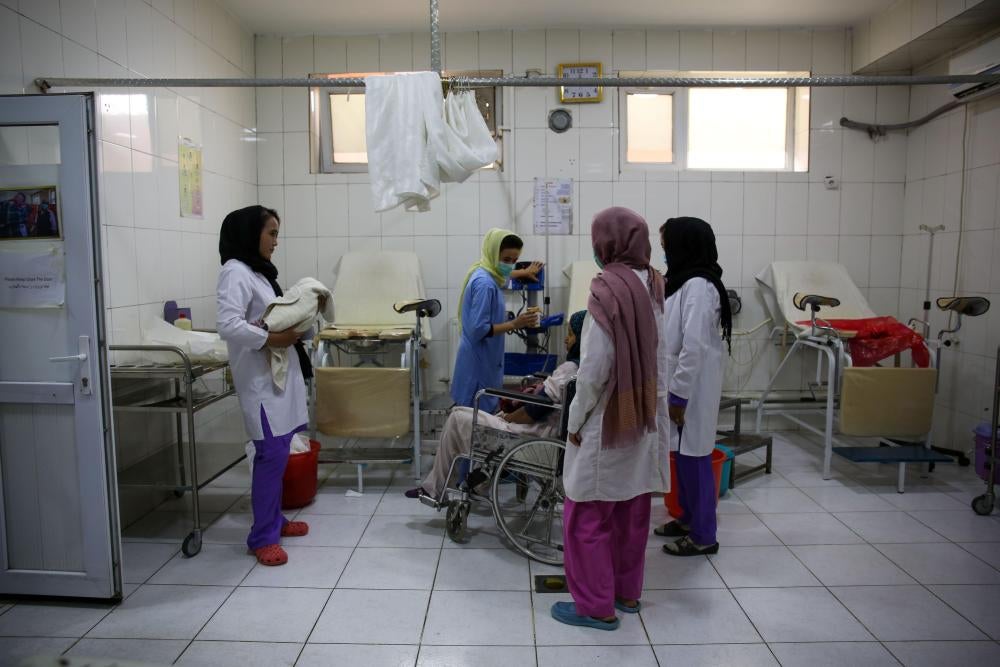
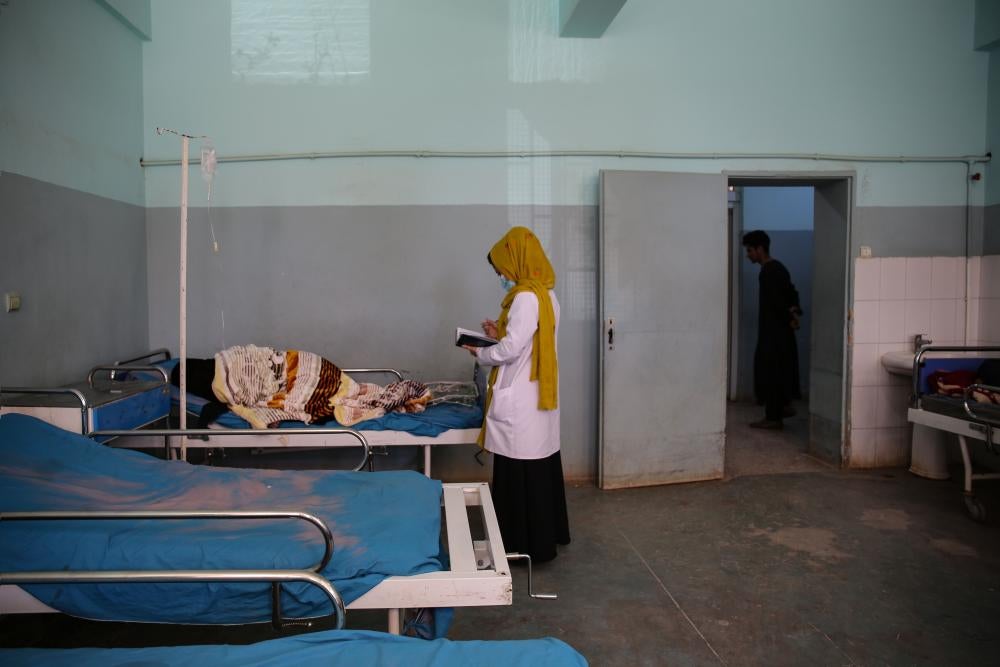
Human Rights Watch visited health facilities in Kabul, the capital, and interviewed 34 women about their experiences seeking and receiving health care, 18 people working in healthcare delivery, 4 donor entities, and additional experts including international and nongovernmental organizations (NGOs).
What emerged is a picture of a system that is increasingly unaffordable to the estimated 61 to 72 percent of Afghan women who live in poverty, and one in which women often have more children than they want because of lack of access to modern contraception; face risky pregnancies because of lack of care; and undergo procedures that could be done more safely with access to and capacity to use more modern techniques.
This is a critical moment in Afghanistan. In addition to the announced US withdrawal, other member countries of NATO also plan to withdraw their forces in a manner coordinated with the US. While the US withdrawal does not require any conditions to be met, some international donors have increasingly sought to make provision of development assistance conditional based on factors that include respect for human rights and women’s rights specifically. People interviewed by Human Rights Watch expressed fears that the Taliban would obtain increasing control over the lives of Afghans or that the already-high level of violence in the country would escalate.
Both scenarios—growing Taliban control and rising levels of violence—have implications for donor support to Afghanistan, including for women’s health. Donors and organizations delivering services described being locked in a waiting game, with donors unwilling to make firm commitments, and hedging on whether they will be able to fulfill existing commitments until there is greater clarity on the political and security situation. This uncertainty reflects the major challenges that already exist in delivering services in Afghanistan.
It is crucial that donors prioritize meeting the urgent needs of Afghans—including those of women and girls for health care. Donors and NGOs have learned many hard but valuable lessons about delivering services amidst deep insecurity and in areas under Taliban control. The US and other troop-deploying countries in Afghanistan should assess the need for aid and their commitment to providing it separately from the decision to withdraw their forces. They should fully appreciate the depth and urgency of the needs in Afghanistan, and not use political and security developments to justify disengaging when the need for international assistance is greater than ever.
Recommendations
To the Afghan Government
- Continue prioritizing support and reform of the health system and include a strong focus on women’s health.
- Increase monitoring and strengthen accountability measures, such as complaint mechanisms to reduce and end corruption in the health sector.
- Develop and implement a plan to provide comprehensive sexuality education to all Afghans, including women and girls, and people who do not attend formal education.
- Expand access to psychosocial support and mental health services, including a focus on providing these services, in a gender-sensitive manner, to women and girls.
- End the requirement that a husband must consent to his wife accessing contraception.
- Track the provision of health services in provinces and districts, including: the number of health facilities closed, the reasons for closure, the number of health facilities operating, the number and gender of staff in different roles present in those facilities, the number and gender of patients seen in those facilities, and services provided, and regularly publish this data.
To the Taliban
- Support provision of health services and reform of the health system and respect the right of everyone, including all women and girls, to have full access to all health services.
- Permit and facilitate education for girls and women to ensure literacy about family planning and health, and support training future female health workers.
- Do not threaten, attack, or extort resources from health workers or facilities.
- Permit comprehensive sexuality education and full access to modern contraception.
To International Donors, including the US, EU, UK, and Canada
- Sustain or increase support to the Afghan health system, particularly women’s health care, and continue this support regardless of political or security developments.
- Commit to using innovative approaches to deliver health services in insecure areas, using lessons learned from Afghanistan and elsewhere.
- Monitor provision of health care closely, using third-party monitors, to guard against corruption and other barriers, and ensure quality of services and that the services are reaching patients.
- Consider supporting preventive and specialist health services, including those most needed by women and girls, and make decisions about funding priorities and program design in full consultation with Afghan healthcare experts.
To the United Nations Assistance Mission to Afghanistan
- Track and report on the availability of essential services such as health care including indicators such as the proportion of female staff and patients, and number of maternal and infant deaths, in at least a sample of the country.
Methodology
Human Rights Watch conducted research for this report in March and April 2021. The research included 56 in-person interviews in Afghanistan plus 7 additional interviews with experts via video conferencing. 34 interviews were with Afghan women about their experiences of seeking and receiving health care. 18 were with Afghans working in the health sector, ranging from the minister of public health to a hospital cleaner, and including doctors and people working in management, midwifery, nursing, and physiotherapy, most of whom we were able to interview during visits to health facilities. The rest were with donor agency officials and with other experts on the health sector or women’s rights in Afghanistan.
Interviews with women about their experience accessing health care and with healthcare workers were mostly conducted in Dari through interpretation. Interviews with experts were in a mix of Dari and English. Interviewees were advised of the purpose of the interview and how the information would be used and gave informed consent. They were not provided any compensation. Women interviewed about their experiences were interviewed individually. Several interviews with health workers were with more than one person at a time. Interviews with experts were often with multiple people from the same organization.
Names of some women interviewed about their health histories were replaced with pseudonyms at their request to protect their privacy. Some health workers also requested that their name be withheld. When quoting health workers speaking critically of facilities in which they worked we have withheld their names to avoid possible retaliation. For security reasons we have also withheld the names of people speaking critically of the Taliban.
The exchange rate at the time of the research was US$1 = 77 Afghanis (Afs); we have used this rate for conversions in the text.
I. Falling Donor Support for Health
Donor funding for Afghanistan is declining across the board. Resources for the health sector are falling at a time when there is a huge need to expand and reform related services.
In 2013, for example, member countries of the Organisation for Economic Co-operation and Development's (OECD) Development Assistance Committee (DAC) contributed US$141 million to health and population assistance in Afghanistan.[1] In 2019, the latest year for which figures are available, that figure was $105 million—a drop of some $36 million, or 26 percent of total funding.
“Success is not possible without international support, but we have problems with sustainability,” said Afghan Acting Minister of Public Health Wahid Majrooh. “We have a lack of resources to sustain progress now, let alone to improve the system…. The areas they are supporting is declining and the amount they are providing is declining. Health is still on the agenda, but we are being pushed toward self-sufficiency.”[2]
But the Afghan government has little ability to move toward self-sufficiency in the short term. Over 75 percent of its budget comes from international donors—in particular the United States, European Union institutions, Germany and the United Kingdom.[3] In 2020, the country’s sustainable domestic revenues fell 2.8 percent compared to 2019, due in large part to the economic downturn resulting from the Covid-19 pandemic.[4]
It is difficult to compile exact total figures on donor assistance as not all figures are public or comparable, and pledges may differ from disbursements. But it is clear that both funding to Afghanistan overall and funding to the health sector specifically have been in decline and continue to be. As donor funding to the health sector falls, already-inadequate services are further deteriorating, and this problem is likely to worsen.[5]
At a November 2020 conference in Geneva, Switzerland, one of periodic donor conferences for Afghanistan, donors pledged about $2 billion less for the period from 2021-2024 than they had for 2016-2020, a reduction of up to 20 percent.[6] This came at a time when the United Nations Development Programme (UNDP) had calculated that, due to the impact of the Covid-19 pandemic, Afghanistan would need an increase of 30 percent in international aid “to maintain the level of government expenditure initially planned in the IMF [International Monetary Fund] projections.”[7]
Aid has been falling for years. Overall development assistance to Afghanistan according to OECD DAC was $6,862 million in 2013, and $4,053 million in 2019.[8] The US, an OECD DAC member, provided a total of $16,748 million in assistance in Afghanistan in FY 2010, versus $3,120 million in FY 2021.[9] Donors in Kabul confirmed that support is declining, saying that while a few donors, such as the EU, have pledged to maintain their prior funding level, others are cutting their funds significantly. No major donors are significantly increasing their aid to Afghanistan.
In 2019, the World Bank reported that Afghanistan spent $8 per person per year on health, with on-budget health expenditure representing about 1.5 percent of Gross Domestic Product (GDP).[10] This contrasts with global benchmarks recommending that countries should spend amounts ranging from over 5 percent of GDP and up to 6 to 7 percent of GDP on health.[11]
Falling aid is having real consequences. Although statistics are not available, interviewees working in the health sectors said that within the Ministry of Public Health, including health facilities, the number of technical advisors, funded by donors and responsible for helping to drive reforms, has shrunk significantly, leaving many reforms stalled.[12]
The director of a government hospital providing maternal health services said it previously provided medications and supplies to patients for free, but this ended about three years ago due to decreases in the hospital’s annual budget over the last seven years, totaling about a 30 percent decline. It is now in a worse position, as international aid for the hospital ended several months ago and the budget for the current fiscal year has been cut by at least 15 percent. When Human Rights Watch visited in early April 2021, the staff had not yet been paid their salaries for over three months, and hospital midwives said they were told their salaries might be cut from the current 13,000 Afs ($169) to 7,500 Afs a month ($97).[13] “I feel bad for myself that I am a midwife,” one said. “I regret this choice.”[14]
Most international support to Afghanistan’s health sector flows through a pooled fund, the Afghanistan Reconstruction Trust Fund, administered by the World Bank. Sehatmandi, a project that the bank administers and the Health Ministry implements, supports the provision of health care through two frameworks, the Basic Package of Health Services and the Essential Package of Hospital Services.[15] The program, with a budget of $600 million, is set to run until June 30, 2022 (having begun in 2018), and is implemented primarily through contracts with national and international NGOs.[16] Sehatmandi results indicators, which are targets and are used to measure the efficacy of the project, include “Contraceptive Prevalence Rate (modern methods)” and “Births attended by skilled health personnel.”[17]
II. Incomplete System: Women’s Limited Access to Health Care
“I would like four children—if we stay alive in Afghanistan.”
—Massouma, age 27, nine months pregnant with her second child.
Every day, millions of women in Afghanistan go without health care and information about their health that most of the rest of the world takes for granted. The life expectancy at birth of Afghan women is 66 years[18]—providing better health care would allow many Afghan women to lead longer and healthier lives. Delivery of health services for women and girls remains far below international standards, and progress on some key indicators is stagnating or reversing.
Women’s right to equal access to health care services is a critical element of the right to health guaranteed under international law. The International Covenant on Economic, Social and Cultural Rights provides equal rights to the “highest attainable standard of physical and mental health.”[19] The Convention on the Elimination of All Forms of Discrimination against Women guarantees this right to all women and girls, including those living in rural areas.[20] The United Nations Committee on Economic, Social and Cultural Rights, in its general comment on the right to health, has stated that:
The realization of women’s right to health requires the removal of all barriers interfering with access to health services, education and information, including in the area of sexual and reproductive health. It is also important to undertake preventive, promotive and remedial action to shield women from the impact of harmful traditional cultural practices and norms that deny them their full reproductive rights.[21]
Afghanistan has 4.6 medical doctors, nurses, and midwives per 10,000 people, far below the threshold for critical shortage of 23 healthcare professionals per 10,000 people set out by the World Health Organization.[22] Distance from health facilities remains a problem for a significant proportion of the population; almost 10 percent of people cannot reach a health facility within 2 hours and 43 percent must travel more than a half-hour.[23] Lack of access to adequate care drives Afghans to spend $285 million a year on medical tourism, mostly in Pakistan and India, draining funds from the sector.[24]
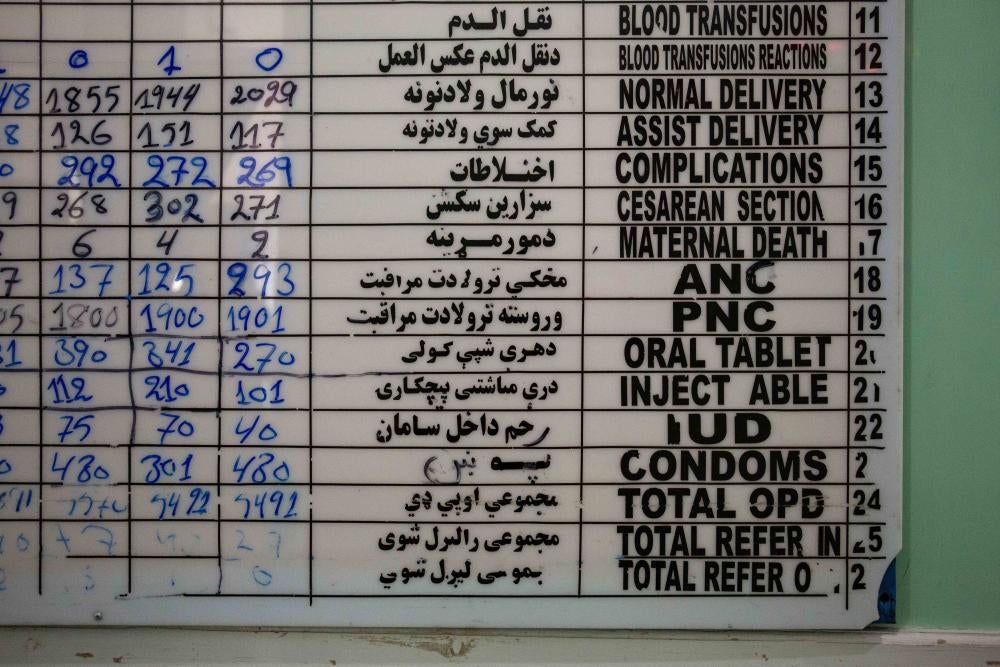
The maternal mortality rate declined from 1,200 per 100,000 births in 2002 to 638 in 2017, an impressive improvement mainly attributable to advances in the delivery of basic health services including skilled attendance of deliveries.[25] However, 638 deaths per 100,000 births still puts Afghanistan in a category the United Nations International Children's Emergency Fund (UNICEF) calls “very high.”[26] Afghanistan is the only country in Asia in this category.[27] UNICEF estimated there were 7,700 maternal deaths in Afghanistan in 2017.[28] By contrast, the United Nations documented 3,438 civilian deaths due to military attacks the same year.[29]
The 2018 Health Survey found 59 percent of deliveries were with skilled attendance, and found that this figure, like the one for prenatal care, had stalled or slightly reversed, particularly among women in deepest poverty.[30] The experience of Muraweet, now 40, and married at age 10, is typical. She had no prenatal care during the first seven of her nine pregnancies, because she could not afford transportation, and she gave birth to the first seven children at home, unattended.[31]
This report does not examine children’s access to health care, but it is worth noting that Afghanistan’s rate of infant mortality, while also significantly improved since 2001, remains 47 per 1,000 live births, high above the global rate of 28.[32] Most health facilities in Afghanistan have little if any capacity to provide emergency care to newborns. One hospital visited by Human Rights Watch had ten incubators, but five were broken and the hospital was not able to repair them. “We lose a lot of babies—in one week usually two or three,” a midwife at another government hospital said. “Mostly kids [who do not survive] are premature, and we don’t have facilities to treat them so the baby will be alive for a few minutes.”[33]
Many of those seeking women’s health care, including maternal health care, are girls. One factor contributing to Afghanistan’s high rate of maternal mortality is the prevalence of child marriage. 35 percent of girls in Afghanistan marry before age 18, and 9 percent before age 15.[34] Many of the women interviewed for this report had married as children; among them the youngest age of marriage was 10. Afghan law sets the minimum age of marriage at 18 for men and 16 for girls, which violates international human rights law prohibitions on discrimination based on gender, and permits girls to marry at age 15 with permission from their father or a court.[35] Child marriage is associated with early and closely spaced pregnancies, which can have serious health consequences, including the risk of death, for pregnant girls and their babies. In 2017, the government launched a national action plan to end child marriage, but little progress has been made on implementing this plan.[36]
Through interviews with women about the experiences of seeking and receiving health care, and with health workers and experts, Human Rights Watch documented major barriers to women accessing services, even in the capital, Kabul, where most of the best quality services in the country are concentrated.
Women and girls outside of Kabul face greater barriers and scarcity of services, and in rural areas the situation is even more dire.[37] In 2014, the World Health Organization reported that Afghanistan had only 1.9 doctors per 10,000 people, and that the number of doctors per 10,000 people varied from a high of 7.2 to a low of 0.6 in the least served areas.[38] Rural facilities are often understaffed or have few or no female staff. Insecurity due to fighting between the government and insurgents creates risks for health workers, contributes to understaffing, especially by female workers, and deters women and girls from seeking care. Health facilities outside cities have limited capacity to treat serious conditions and often refer patients to urban hospitals.[39]
“If there is no fighting it takes five hours. If there is fighting, we don’t know,” said Zahra, 25, who traveled from her home in Ghazni to a hospital in Kabul to give birth to her second child. She has high blood pressure and doctors at the government hospital in Ghazni said they could not treat her. “They thought it might not be a normal delivery and the baby might need special care and they cannot provide that,” Zahra said. She had had the same difficulty with her first pregnancy and was delayed for several hours by fighting on the road while making the same journey, before arriving in Kabul for an immediate emergency cesarean section (C-section).[40]
“There is no doctor in [my area of] Ghorband [an insecure district within Parwan province]—there is fighting in that area, it is a Taliban area,” said Shirin Gul, 65. She had already been displaced from her village when she started experiencing vaginal bleeding and felt a rapidly growing lump in her groin. “There was fighting—they burned the houses including mine and stole everything we have and destroyed our garden,” she said. She traveled to a Kabul hospital where doctors operated and removed a 2.5-kilogram uterine mass.[41]
“The lack of access to health professionals in the provinces and districts is still there,” said Hosna Jalil, deputy minister of women’s affairs. “Services are concentrated—especially health services—in major cities. We don’t have access or quality in all provinces.”[42]
Jalil raised particular concern about lack of mental health services, especially for women.[43] Globally women are more likely to experience some common psychosocial disabilities (mental health conditions), such as depression and anxiety.[44] More than half the Afghan population, including many survivors of conflict-related violence, experience depression, anxiety, and post-traumatic stress, but fewer than 10 percent receive adequate psychosocial support from the state.[45] Women and girls face particular barriers in accessing services.[46] One woman, who had just given birth, described trying to take her own life seven times during the late stages of her pregnancy after she faced domestic violence, a loved one was murdered, and another diagnosed with cancer.[47]
The Ministry of Public Health says only about 26 cents per capita is spent on mental health.[48] While the mental health budget has increased since 2006, it remains below the $2 per capita the World Health Organization has determined is an appropriate investment for mental health systems in low-income countries such as Afghanistan.[49]
The Asia Foundation has reported that some 89 percent of Afghans have mild to severe disabilities,[50] and women and girls with disabilities face intersecting and compounding forms of discrimination that often block them from accessing assistance, including health care.[51]
The Covid-19 pandemic has worsened women’s access to health care in multiple ways, including by plunging many families deeper into poverty and reducing the resources available to the government to support health care.[52] “I think before Covid it was getting better,” a Ministry of Public Health senior official said. “But with Covid some doctors got sick and then people were afraid to visit hospitals or clinics until there was an emergency because they were afraid of getting sick.”[53]
Barriers to Women and Girls Accessing Health Care
Impact of Insecurity
Afghanistan’s armed conflicts have undermined women’s access to health care for decades and continue to do so. The World Health Organization has estimated that up to 3 million Afghans were deprived of essential health services in 2020 alone due to closure of health facilities by parties to the conflict, including the Taliban, groups affiliated with the Islamic State of Khorasan Province (ISKP, an affiliate of the Islamic State, also known as ISIS), and Afghan government forces.[54]
A particularly horrific example was the May 2020 attack on a hospital maternity ward operated by Médecins Sans Frontières (Doctors Without Borders, MSF), in which attackers systematically killed 24 people, including mothers, women in labor, newborns, a midwife, and 2 children under 10, leading MSF to close the ward.[55] The attack has not been claimed. In 2020, the United Nations Assistance Mission in Afghanistan (UNAMA) verified 90 attacks impacting healthcare delivery, 71 of which they attributed to the Taliban and 9 to pro-government forces.[56] Eight health personnel were killed, eleven injured, and thirty-six abducted in these attacks. The Taliban also forced the closure of dozens of health facilities after health providers refused to comply with Taliban demands for assistance for their fighters.[57]
Health facilities and workers have often been caught in the middle of the conflict. “The Taliban are using health centers as safe areas,” a government official said. “Health workers can’t travel across battle lines because then they are suspected of being infiltrators. This is part of why rural areas are so underserved in terms of health care, especially in areas like Helmand.”[58]
Health facilities have often been forced to close due to insecurity. Officials told Human Rights Watch that usually they do not close permanently but on and off during periods of heightened insecurity, sometimes for many months.[59]
The Taliban often distinguish between health workers in the private sector and those working for the government, whom they oppose more strongly. “We faced a lot of war—pieces of bodies fell on our roof during explosions,” said a doctor in reference to the period when the Taliban were in power. “But the Taliban were respecting women doctors. I was working privately. But people working for the government—they were killing them, even the doctors.”[60]
A government doctor described receiving a threat from the Taliban who accused her of cooperating with foreign forces.[61] The fact that the Sehatmandi program is implemented through NGOs may help to protect the services and workers, as it gives them some distance from the government in the Taliban’s perspective.
The Taliban sometimes forces health workers to assist them. “My husband is also a doctor,” a doctor from a Taliban-controlled area of Kapisa said. “When a Talib [Taliban member] is injured, they ask him to come and provide treatment. If he goes, he has a problem with the government. If not, he has a problem with the Taliban. We lied many times and said he’s not home. But now we think they know we are lying.”[62]
The Taliban have increasingly sought to impose “taxes” and regulate organizations working in areas they control, including NGOs.[63] NGOs delivering services have long been able to reach accommodations with Taliban commanders on a local level to ensure that service provision can continue. But as the Taliban expand control these agreements are becoming broader and more formalized.[64]
Contested areas and areas under Taliban control have also been affected by residents lacking livelihoods. This harms access to care because, as discussed below, even when obtaining “free” government services, people need to pay for transportation and often for medicines and supplies, which can cost significant amounts—amounts out of reach for people living in poverty.
A doctor from Kapisa said of her area:
It’s Taliban-controlled—people are poor, there are no jobs. There are a lot of pregnancies…. Clinics are far from where they live, so often they die or the baby dies…. People don’t even have money for transport to the center, to a government hospital, and you still have to pay for medicines at the government hospital. So, many give birth at home. Some borrow money, or if they can’t borrow, they might lose the baby or the mother or both.[65]
Farzana planned to go to back to the MSF hospital for a tubal ligation—a procedure that prevents pregnancy by blocking a woman’s fallopian tubes indefinitely—36 days after her sixth child was born but decided to delay for a few days because of worries over Covid-19. On the 36th day, the MSF hospital was attacked. “I am scared of hospitals after that attack,” she said, explaining that fear over what happened, and other recent violence in Kabul, had led to her delaying vaccinations for her children.[66]
“Concerns regarding safety determine access,” said Matt Rubin, author of a section on health in a recent report by the US Special Inspector General for Afghanistan Reconstruction on women’s rights.[67] “Insecurity is deterring people from working in clinics, and that leads to greater staffing gaps, especially among female staff. Even if a clinic is there—within the one-mile figure—it is almost moot because quality of care is increasingly an issue.”[68] For cultural reasons, many women in Afghanistan are only willing to be treated—or are only permitted by their families to be treated—by female health workers.
Insecurity also influences choices about family size. “In your country you have security, but here there is fighting,” said a doctor in a maternal ward explaining women’s decisions. “If I give birth to four kids, two might die in explosions—I might lose them…Something might happen to one. And I need one to pray for me.”[69]
Cost of Care
Many women and girls simply cannot afford health care. Poverty is alarmingly high in Afghanistan and rising dramatically. The percentage of people living below the national poverty line in Afghanistan had already risen from 38 percent in 2011 to 55 percent in 2016.[70] The World Bank estimated in mid-2020 that the country’s economy could contract by 6 to 7 percent in 2020 due to the Covid-19 pandemic, and poverty was likely to rise to between 61 and 72 percent.[71]
The GDP per capita was $507 in 2019, prior to the Covid-19 pandemic, and salaries are extremely low.[72] So many people in Afghanistan are so poor that even costs that seem small lead many people to go without needed care. Women face particular barriers as they are less likely than men to have access to their own money or control over the family’s financial resources.[73]
Even when care is free, or almost free, as in the government hospitals where the only official fee is a 20 Afs ($0.26) registration fee,[74] the reality is that, as discussed below, there are often costs to receiving health care that are difficult or impossible for many to afford. Increasingly, as budgets have been cut, patients must pay for all medications and supplies used in their care—something Human Rights Watch found at all government health facilities we visited. When a patient arrives at a government hospital, for example a woman in labor, they are typically instructed on what to purchase and sent out with a prescription to a nearby pharmacy. These supplies include items like gloves, gauze, catheters, scalpels, sterilizing fluid, and all medicines.
“The patients are providing the medicines and the consumables themselves,” the director of a government hospital said. “Five years back, patients would come without even 100 Afs [$1.30]. Now in some big operations they spend 5,000 Afs [$65] for care—for drugs, consumables.” The director acknowledged that this was happening at a moment of rising poverty. “Now the clients don’t have the money. And we also in the hospital don’t have the money.” He said on five occasions in recent years the hospital ran out of anti-coagulant drugs and was unable to find them for sale or direct patients to a place where they could be found. [75] Government health facilities are also often unable to perform needed diagnostic tests, and instead send patients to private labs, where they must pay costs that are often around 1,000 to 2,000 Afs ($13 to $26) per test.[76]
Freshta, 38, from Shamali, said her husband had borrowed 15,000 Afs ($195) to pay for the travel expenses and medicines and supplies she needed to receive surgery for ovarian cysts at a government hospital in Kabul. “This is the first time in a hospital in my whole life,” she said. “I thought everything was free, but I had to pay for gloves, food, medicine, and go outside the hospital to do blood tests, and pay for that.”[77]
“When I was pregnant last time, they said it would be a C-section, and I was calling for three days to try to borrow to pay for it, but everyone refused,” said Sediqa, 33, a mother of four. “It costs 15,000 Afs to 20,000 Afs [$195 to $260] for a C-section—you have to pay for transportation, food, medicine, anything for the mother and child.”[78]
Zarmina, 27, had gone to the hospital that day in labor with her fourth child. She had never received prenatal care during any of her pregnancies because her family could not afford the cost, and she was worried that day that she might need a C-section. “I already bought gloves and other things needed for today—it cost 2,000 Afs [$26],” she said. “If I need a C-section, I have no more money. I had 2,000 Afs and I spent it all.”[79]
Officials in the health ministry confirmed that the government previously had more ability to provide supplies to health facilities but as donor funding declined this capacity has shrunk, and sometimes disappeared.[80] “We cannot have medicines from the government because there is no budget for it,” the head of a government hospital explained. “Patients think that we have medicine but won’t give it. Family members of patients ask but we can’t provide this…. Our patients are very poor.”[81]
Transportation costs alone put care out of reach for many women. Farzana lives in one of the districts of Kabul, and it takes her an hour by car to reach the government hospital where she gave birth to several of her children. She heard from a neighbor about a government clinic where she could get affordable prenatal care and went there every month during two of her six pregnancies, but because she could not afford a taxi, which might have cost about 300-500 Afs each way ($4-6), each trip instead involved a 40-minute ride on public transport, at a cost of about 40 Afs ($0.52) followed by a one-hour walk, each way. “That’s the closest that public transport goes,” she said.[82]
Some services are available only, or more readily, in the private sector, but only for those who can pay. Health workers who work in government facilities often run a private clinic on the side and attract patients from the government facility into their private services with the promise of better care.[83]
Farzana’s second son was unwell after she gave birth to him at a government hospital. The staff at the government hospital told her to take him to a private clinic, which she did but the clinic wanted to keep him for 14 days, at a total cost of $649. Her family could not afford that, so she took him home after seven days. With Farzana’s sixth pregnancy, she had difficulties with water retention and went to a private clinic for help but fell three times in the snow walking there only to find that it cost 2,100 Afs ($27) and she only had 500 Afs ($6). “I didn’t know it would be so expensive,” she said. Her extended family lives on an income of about 10,000 Afs ($130) a month.[84]
Corruption and demands for bribes can add additional costs, as recently appointed Acting Minister of Public Health Wahid Majrooh acknowledged, saying, “Recent allegations of corruption worsened the situation—people question how resources are used.”[85] The ministry has faced both longstanding allegations of corruption and a 2020 investigation into misuse of funds provided to fight Covid-19.[86] Corruption has also been a barrier to delivery of reforms, including patients being asked to provide under-the-table payments to access services.[87]
“In the government hospital they don’t care about you, so you have to pay to get good care,” said Farzana, who said when she gave birth in a government hospital the midwives demanded 2,000 Afs ($26) and she felt she had to pay it or risk mistreatment.[88]
Poor Quality Care and Difficult Conditions for Health Workers
Women sometimes seek private care after experiencing what they perceive as poor-quality care in government facilities. Human Rights Watch interviewed Atifa, a mother of nine children, at a private hospital where she had sought treatment after her C-section incision became infected. She had given birth in a government hospital six days earlier but was unwilling to return there for help because of how she felt she had been treated, even though her family struggled to afford private care. “My operation took three hours—it should have taken one hour,” Atifa said. “The nurses were young—they didn’t care for me. I was awake, I could see them. When I said, ‘What are you doing to me and my body?’ they gave me an injection and then I couldn’t follow anything.”[89]
Harina, 32, was left with obstetric fistula after her second delivery in a government hospital and felt it was the result of poor care. She had an operation to repair the damage in a private hospital, at a cost of 25,000 Afs ($325) and gave birth to her third child in the same private hospital, but for her fourth birth she could no longer afford private care and returned to the government system.[90]
A Human Rights Watch researcher observed a staff member at a major government-run hospital in Kabul speaking abusively to a room full of post-delivery patients in a hospital, mocking a patient who could not speak Dari,[91] and refusing to inspect that patient’s incision which she worried might be infected. Conditions in some facilities Human Rights Watch visited were extremely crowded for both staff and patients, with two patients sometimes crammed into a narrow single hospital bed, with heads at opposite ends. There was also poor cleanliness in some facilities with dirt and garbage on the floors.
Health workers work under extremely difficult conditions. Midwives in a government hospital described working 24-hour shifts, without sleeping or sufficient food, and without access to a private room or changing facility, in teams of 4, each team managing about 45 to 50 births per shift.[92] A midwife in a managerial role said on her 10,000 Afs ($130) a month salary she supports seven family members. When she became ill with Covid-19, she and her immediate family members lacked resources to quarantine anywhere except in a tent outside the home of their extended family, in winter; conditions were so harsh that her infant nephew died.[93] Healthcare workers have had limited access to personal protective equipment during the Covid-19 pandemic, and an online survey of more than 900 healthcare workers found that 85 percent of healthcare workers had tested positive for the virus.[94]
Family Pressures, Gender Inequity, and Lack of Autonomy for Women
The World Economic Forum in 2021 ranked Afghanistan last on its index of 156 countries in order of their level of gender equality.[95] The country’s deep gender inequity is reflected in decision-making and power structures within families based in culture and law that make it harder for women and girls to access health care. “Women depend on their husbands. They don’t have independence and their own money,” said Dr. Najmusama Shefajo, head of the Afghanistan Society of Obstetricians and Gynecologists (AFSOG).[96]
“Families don’t allow them to go [to health providers],” a senior health ministry official said. “They think pregnancy is a normal condition, and that it doesn’t need a doctor for pre- and postnatal care and even for delivery. They say it’s best to deliver at home. This is a cultural problem.”[97]
Many families in Afghanistan prefer sons to daughters, because sons are expected to remain with and support their parents, while daughters are expected to marry and leave, and this plays a role in decisions about the number of children women will have. The preference for sons is driven by practical considerations in a country with no social safety net. Majan, 50, has 11 children. “I wanted three sons and two daughters,” she said. “But my daughters were oldest. I kept having children to have sons. Daughters will marry men and be part of another family. It’s our sons who look after us when we are old.”[98]
The preference for sons may also influence decisions about health care. “Some people come for an ultrasound and then take her to the doctor [for prenatal care] if it’s a boy and not if it’s a girl,” Dr. Shefajo explained.[99] Women often face pressure to give birth to boys.[100]
Gaps in Available Healthcare Services for Women and Girls
Lack of Information and Public Awareness about Sexual and Reproductive Health
Many women and girls struggle to access even the most basic information about their bodies that they need to be able to make informed choices about their health, including reproductive choices. Social stigma against discussing issues related to sexuality contributes to this, as do low rates of education and literacy among women and girls. But the public health and education systems should also do better at providing this information.
Almost none of the information that should be taught to all children as part of comprehensive sexuality education is included in Afghanistan’s national curriculum. At the high school level there is a brief mention of reproductive anatomy and biology, but even for children who reach this grade level—and most children, especially girls, never reach high school—teachers often skip that material.[101] An estimated 40 percent of primary and lower secondary school-age children do not attend school, and by lower secondary school, ages 12 to 15, 66 percent of girls, and 40 percent of boys, are out of school.[102] One interviewee, 32, who was taught it said: “They only mentioned, ‘The sperm does this—this is how the baby is made.’ We had no clue how does this work, and what is sperm made of?”[103] Other essential topics—such as healthy relationships, consent, menstruation and menstrual hygiene management, contraception and family planning, and lesbian, gay, bisexual and transgender (LGBT) concerns—are entirely absent.
“We can’t inform people about sexual health,” a health ministry official said. “It’s sensitive, so we can’t talk about it. But every person has a right to this information.”[104] A health expert said that a video prepared by the ministry on proper use of condoms and posted on social media several years ago received a strong backlash and the ministry removed it from circulation.[105]
Some women said health workers discussed contraceptive methods with them after they gave birth, and some began using modern contraceptive methods as a result. But others said they had never received this information, and had been unable to find information, and many described themselves as having had more children than they wished because they lacked the means to prevent pregnancy.
Others said they learned about options for contraception from television or social media information provided by the health ministry.[106] Some described learning about sexual and reproductive health by searching on the internet and finding information from Iranian websites, or from Facebook posts.[107] Low literacy rates among women (under 30 percent)[108] and low access to the internet resources for women and girls (for example, as of 2016 only 14 percent of Afghan Facebook users were female) contribute to it being hard for women and girls to access health information online.[109]
“Young people at [universities] are talking about this—they can speak on social media, but they could not say it out loud,” said Lima, a university student. “People on social media translate from foreign sources.” The lack of information is so profound that many girls have no information about menstruation before they experience it. “I was scared when I got my period,” said Lima. “At first, I was just sitting on the toilet waiting for it to come out, for 10 minutes. It wasn’t coming out … I didn’t even know to use a pad.”[110]
“I have had nine pregnancies in total, but the information I have about sex is like a 14-year-old girl—I don’t know much,” said Farzana. She has struggled to access effective forms of contraception and had more children than she wanted, but says it is hard for women to share this information with each other, even within families: “It’s a taboo to talk about.”[111]
Acting Minister of Public Health Wahid Majrooh said the ministry, on orders from President Ashraf Ghani, is developing a new national strategy on family planning, expected to be completed by mid-2021, seeking to reduce the country’s fertility rate, which in 2018 was 5.1 children per woman.[112] The minister emphasized that reducing the birth rate is a national priority: “The current rate is unacceptable.” He said the strategy will draw lessons from what the government sees as successful efforts in the region that might be suitable for adaptation to Afghanistan’s cultural context, and will include a plan for teaching about health, including family planning, in schools. “The plan will be contextualized in culture and values, and will partner with community leaders,” he said. “We have to convince society that women are not just for delivery.”[113] Because nearly 70 percent of women have never attended school, measures to provide information both in and out of schools will be crucial.[114]
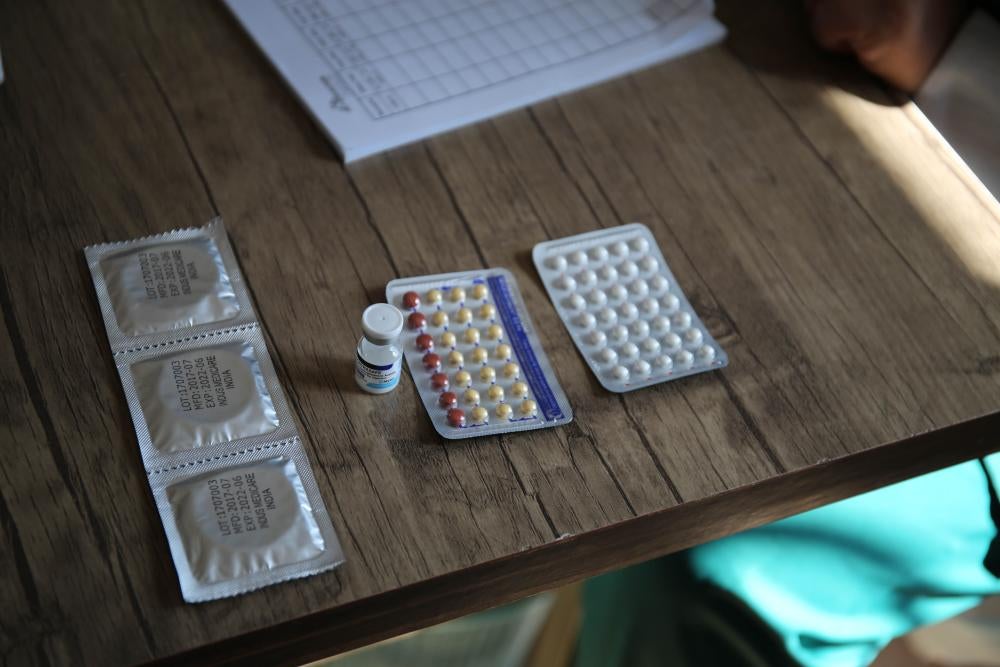
Unmet Need for and Low Use of Modern Contraception
In 2018, 17 percent of Afghan women or girls ages 12-49 with a live birth in the preceding 2 years who had ever been married reported using modern contraceptive methods.[115] This was up from 10 percent in 2003, but progress in this area has leveled off.[116] Afghanistan’s rate of unmet need for contraception, meaning “those who are fecund and sexually active but are not using any method of contraception, and report not wanting any more children or wanting to delay the next child,” is 25 percent.[117] Both of these figures compare unfavorably with other countries in South and Central Asia where rates are closer to 28 to 62 percent.[118]
Access to contraception is particularly critical as Afghanistan restricts access to abortion. Abortion is permitted only when necessary to save a woman’s life, and under other circumstances is punishable, including by prison terms of up to five years.[119]
Some healthcare professionals may not support contraceptive use or may see it as appropriate only after a woman has already had several children. A doctor in the health ministry explained that encouraging women to use contraception is sensitive, and that the ministry cannot instruct healthcare professionals, even those implementing government programs, to do so. “We can just encourage [contraceptive use] generally…. But we cannot force midwives or doctors to have this conversation with families.”[120] The director of hospital agreed: “Some of our doctors have religious minds and they also oppose contraception. But we tell them God will be happy with you.”[121]
Many of the women interviewed described trying and discontinuing forms of modern contraception because of side effects. Several said they felt their mental health conditions were exacerbated when they took pills or injections, or they feared permanent effects on their fertility, or that they had heard it was necessary to eat well while taking birth control pills and they could not afford healthy food.[122] Others became pregnant even though they believed they were using contraception correctly. Better counseling and public information about contraception, as well as incorporating information about family planning into the school curriculum, could resolve some of these difficulties.
Women and girls’ access to contraception is also constrained by health facilities that require a husband’s consent before providing most forms of contraception. “I have a mental illness and can’t take pills. I don’t do injections. So, the only option is tubal ligation,” said Sediqa, who had given birth to her fourth child three days earlier, by C-section. “I wanted to do it three days ago, but the doctors said we don’t know if you have your husband’s permission, so it was too late. I’ll come back in 37 days with permission. My husband has to sign or give a fingerprint.” Sediqa, who works as a cleaner earning 6,000 Afs ($78) a month, thought her husband would agree: “He can’t even find one meal for himself—I pay for it. So he should agree.”[123]
Managers and staff in several facilities confirmed that husbands’ permission is required for contraception. A midwife explained the reasoning baldly: “Men are more powerful than women in this country and they are the decision-makers.”[124]
Many women interviewed said they had had more children than they would have chosen to. “Within 17 years, I had 13 or 14 pregnancies. It’s a lot of work,” said Atifa, 34 or 35, who has nine living children, a son who died in an accident, and experienced several miscarriages. She said her dream was to have four sons and two daughters. She had tried many forms of contraception, but none worked for her. With injections and pills she said she experienced ovarian cysts, and when she had an intrauterine contraceptive device (IUD) inserted it fell out when she carried heavy loads. She and her husband had not been able to use condoms consistently. “He also doesn’t want more kids, but we’re both shy,” she said. “Give me something so as long as I am alive, I will not get pregnant again. I am tired of this.”[125]
Desperately poor mothers are all too aware of the impact a large family has on their ability to provide for their children. “We are so many people, we give birth to so many children—that’s why we don’t have enough food for all of us,” said Freshta, a mother of seven. “I didn’t do anything in my life, but with my kids I tried to show them the way—to do morning prayers and then go to school.”[126]
Nazifa, 33, married at 15, had 6 children before learning about contraception. “I was happy with four,” she said. She took a contraceptive injection but discontinued it when her period did not come, then had a seventh pregnancy that ended in a stillbirth she attributes to the injection. “My oldest daughter asked me, ‘Why six? Two is enough,’” she said. “If I was coming from a rich family, it would be okay to have more.…[But] I didn’t have the opportunity to study so I want them to have that chance.”[127]
Without access to effective contraceptive methods or abortion, women sometimes use drastic measures to end pregnancy. “I tried my best not to give birth to this one,” Farzana, 36, said of her sixth son, a year old. “I used all the advice everyone gave me, but nothing worked.… They said eat saffron, and Ibuprofen and other strong medicines—500 milligrams of anything. Black seeds. I tried to jump from a height. I tried all of these things, but nothing worked.” Farzana’s family was very poor even before the Covid-19 pandemic and during the pandemic her husband’s work as a tailor disappeared and the family lived mostly on bread and tea. Farzana had no information about contraception until staff in a hospital run by MSF discussed options with her after the birth of her fifth son. She and her husband used condoms after that, but she become pregnant again.[128]
In the absence of effective temporary forms of contraception, a steady flow of women seeks tubal ligation. A doctor at a government hospital in Kabul said they perform 5 to 10 tubal ligations every Monday—for patients who can pay for the medications and gloves.[129]
Low Rates of Accessing Pre- and Postnatal Care
Data from 2018, the last year for which data is available, indicates that 65 percent of pregnant women and girls in Afghanistan have at least 1 prenatal visit, and only 21 percent had a recommended 4 or more visits.[130] Progress on this indicator since 2001 has now stalled or slightly reversed, especially among women from the lowest wealth quintiles, according to the Afghanistan Health Survey.[131] Sixty percent of women and girls have no postnatal care.[132] One government hospital that Human Rights Watch visited had over 1,200 births the previous month, but only 45 prenatal appointments.[133]
Many of the women interviewed had accessed little or no pre- and postnatal care, usually because they could not afford transport to travel to health facilities or the costs at both government and private hospitals, which may be as little as one dollar but are unaffordable for families lacking sufficient food. They often went only if they believed there was a problem, and sometimes due to cost could not even do that. Government health facilities have limited capacity to provide prenatal care, forcing many patients who want comprehensive prenatal care into the private system.
Fawzia, 40, gave birth to all her 7 children in government hospitals, but turned to private clinics for prenatal care. She said if you go to a government hospital for prenatal care, “They do a check-up, but they have no scan, so they send you to another private clinic.”[134] Harina, 32, tried accessing prenatal care at a government hospital but found that she was sent outside to get a scan and blood test and buy supplies and decided to return to the private system even though it cost 700-2,500 Afs ($9-$32) per visit.[135]
One consequence of women and girls going without prenatal care may be undiagnosed or late diagnosis of ectopic pregnancy, which can be life threatening.[136] Sanam, 27, has had 2 ectopic pregnancies and 1 live birth. Both ectopic pregnancies were treated through open surgery; the second one was initially misdiagnosed as a cyst. Sanam’s husband works in a shop and they struggled to afford the 9,500 Afs ($123) they had to pay for gloves, serum, medicine, scalpel, and other supplies for the most recent operation. They also incurred earlier costs when Sanam went to a private clinic where the ectopic pregnancy was diagnosed.[137]
Jamila, over 28, traveled for about 3 hours from Ghorband district in Parwan province to Kabul for treatment after a doctor near her village said it seemed like her pregnancy was “in the wrong place.” Her husband and mother-in-law came with her and had also been staying at the hospital for three days.[138] Some hospitals have a basic room where families of patients who have traveled in from outside the city can sleep.
The director of a Kabul government hospital said that ectopic pregnancy is treated only through open surgery at that hospital. “We have to do surgery for ectopic pregnancy because we don’t have laparoscopic equipment. There is medicine that can be used to treat this, but we can’t always find it in the bazaar.”[139] Capacity to perform laparoscopic surgery could also facilitate safer procedures for fibroids, cysts, and hysterectomies.
Lack of Preventive and Specialty Care
Donors have understandably focused on delivering basic health services, but Afghan experts expressed some frustration on the lack of progress on more specialized and preventive services. “Not as much has been done as we expected,” said Dr. Shefajo of AFSOG. “In 2001 people were going outside the country to get health care, and they are still doing that.”[140]
“There are no routine mammograms or pap smears in the government system—not even for health providers,” an official from the health ministry explained. “We hope to bring this, we tried to raise this [to donors] but they have other priorities.”[141]
“For primary services, there has been an improvement, but there was not the same improvement for tertiary services,” the ministry official said. Tertiary services are specialized consultative health care, usually provided to inpatients on referral from a primary or secondary health professional. “There was less money, and it was not a priority for the international community.” She cited gaps including endocrinology and cancer treatment in women’s health care. Regarding breast cancer, she said, “We can diagnose but not treat, and diagnosis is done in the private sector.” She said only one government hospital in Kabul has mammography and sonography equipment, and one other government hospital has capacity to do surgery and fine needle aspiration; patients are obliged to travel between different private and government facilities to receive care.[142]
Acting Minister of Public Health Wahid Majrooh raised similar concerns: “Due to lack of secondary and tertiary care, people have to travel abroad [typically to Pakistan or India]. This has created a gap between the citizens and the health system. People think that the system can’t meet their needs.” He highlighted lack of capacity to provide advanced diagnostic imaging such as MRI scans and mammography, cancer operations, laparoscopic surgery, colposcopy procedures, and fertility treatment including in vitro fertilization. “This is the minimum needed,” he said.[143]
The health system lacks the capacity to diagnose and treat life-threatening illnesses. Sajida, 26 and married for ten years, had given birth to three children, all of whom had died, two within days of birth and one after three months. “They were smaller than normal, weak, and had heart issues,” she said. She was five months pregnant when Human Rights Watch interviewed her. No one had been able to tell her what was wrong with her children or do anything to help reassure her that the same thing would not happen again. “They told us everything was okay even after the birth,” she said of the private clinics where she had been treated and given birth. “When we lost all three, they said it’s God’s will.”[144] Another interviewee was at a hospital looking after her cousin, 20, who married at age 14 and had one living child but was going through her third full-term stillbirth.[145]
One area of urgent need is fertility treatment. None—for women or men—is provided through the government system, and treatment in the private sector is often poor quality. Maliha, 26, had been married over 7 years and struggled to become pregnant. “I went to 14 or 15 doctors so far,” she said.
I went to doctors and mullahs and traditional healers. The doctors said you have tuberculosis. The mullahs said someone did black magic toward me. The traditional healer said it’s because you are overweight. The doctors gave me medicines. The mullah said bring money and I will find a solution. The female healer said bring a sheep and money and I will do something to solve this.
She said another female healer asked her to bring a chicken and then put the chicken on Maliha’s stomach, and this led to a pregnancy, but it ended in miscarriage.[146]
Access to effective fertility treatment is sought with desperation in part because women and girls may face abuse if they do not become pregnant. Tahira, 23 or 24, has been married for 7 years and had 2 miscarriages and no children. The pressure on her from her in-laws due to her lack of children become so overwhelming that she and her husband moved out and live alone in a rented room without contact with his family.[147]
Zarghona, 30, married 8 years ago and has tried to become pregnant ever since. “People give me names, and I go to doctors. I lost count of how many,” she said, producing a bundle of letters from at least 15 doctors. She had been given a number for a clinic in Kabul and kept it for two months while she waited for the fighting on the road from Ghazni, where she lives, to die down so that she could safely make the journey. “My husband said, ‘If you don’t get pregnant this time, I will marry someone else.’” Polygamy is legal in Afghanistan, and Zarghona said that if she does not become pregnant, she will find a second wife for her husband and they will live together. “I don’t even want to think about it,” she said.[148]
III. Impact on Health Sector of Increased Violence or Taliban Control
There is no end to this war. We lost generations…. My mother used to talk about war when I was a child in Iran, and then I came back to the same war, and now my children are talking about this war.
—Gulchaman, 43, maternity ward cleaner
There is rising uncertainty, and fear of escalating violence or growing Taliban control, as the US is set to withdraw all its troops before September 11, 2021. People interviewed for this report—from women receiving health care to government officials to donors—discussed the risk that in the coming months political instability could lead to rising insecurity or expanded Taliban control, or both. Both scenarios pose risks for women’s access to health care.
Insecurity is already a major barrier to women and girls accessing health care, as discussed above, and greater violence would exacerbate the problem. “I’m not really hopeful about what will happen with the future of this country,” a public health ministry official said. “There’s been a lot of change in this sector in the last 15 years. If the situation gets worse, we won’t be able to have the services we have today.” She described fighting in the 1990s, saying almost all hospitals and midwifery services closed, and even people injured in the fighting could not get care. “I have worries that if that comes again everything might be destroyed.”[149]
Growing Taliban control—for example, through military advances or inclusion in the government—could also have grave implications for women’s health. Taliban officials in Doha, Qatar told Human Rights Watch that there was a need for more health facilities in rural areas, saying that those that existed were largely in cities and areas under government control. They urged NGOs to direct more assistance to rural areas, saying “the needs are dire—women are dying in childbirth needlessly.”[150] However in November 2020, the Taliban issued new regulations requiring all NGOs to register with them in order to provide services in Taliban-held areas. In some areas, Taliban officials have prevented female staff members of NGOs from traveling in districts under their control.[151]
When the Taliban were in power pre-2001, they imposed restrictions on the movement of women and girls that dramatically curtailed their access to health care.[152] One woman described giving birth at home, unattended, during the Taliban time because she was afraid of being beaten if she left the house. “I was scared of them,” she said. “They don’t care if you die.”[153] The Taliban has also generally opposed provision of modern contraception.[154]
As the Taliban have consolidated control over approximately half of the districts in Afghanistan, they established a health policy implemented by provincial and district level health commissions that oversee all healthcare services, which in almost all cases are provided by NGOs.[155] Taliban policies, such as allowing women to travel only with a male relative or an older woman restricts women’s access to health care in these areas, although female healthcare workers provide services at clinics and hospitals, and make home visits to see female patients.
“The Taliban said they will allow women to work,” a midwife at a government hospital said. “If they keep their promises, it shouldn’t be a problem. Otherwise, we have to stay at home and wear a burqa. I hate burqas.” She expressed skepticism about Taliban assurances that women will be able to work if they gained control. “They kill people every day—how can we trust them?”[156]
At least some provision of health care for women and girls should be able to continue regardless of whether the role of the Taliban grows. Hosna Jalil, deputy minister of women’s affairs, made the point that the Taliban did not impose blanket prohibitions on women’s access to health care during their rule, as they did with access to education and employment.[157]
The Afghan government has endeavored to provide health services, and other essential services such as education, across the whole country including in Taliban-controlled areas, although the Taliban may receive credit for such services in the eyes of communities.[158] “Health is a human right,” said the Wahid Majrooh, acting minister of public health. “This sector is impartial—we don’t label people.”[159]
Both scenarios—rising levels of violence or growing Taliban control—have implications for donor support to Afghanistan, including to women and girls’ health. Both donors and organizations delivering services described being locked in a waiting game at present, with donors unwilling to made firm commitments, and hedging on whether they would be able to fulfill existing commitments, until they see what happens on a political and security level in the coming months.
This trepidation is understandable given the volatility of the situation and the major challenges that already exist in delivering services.
But donors should prioritize meeting the urgent needs of Afghans, including the need of women and girls for lifesaving health care. Many hard-won and valuable lessons have been learned in Afghanistan about delivering services even amidst deep insecurity and in areas under Taliban control. Countries that have a military presence in Afghanistan are understandably exploring options to withdraw their troops from Afghanistan and assessing current levels of aid, but they should fully appreciate how deep and urgent the needs are in Afghanistan, and not use political and security developments as a justification for disengaging when the need for international assistance is greater than ever.
Acknowledgments
This report was written by Heather Barr, interim co-director of women’s rights, based on research she conducted with Tamana Ayazi, a consultant to Human Rights Watch. Susanne Bergsten and Erika Nguyen, coordinators in the women’s rights division assisted with proofing, sources, and footnoting. It was edited by Tom Porteous, deputy program director, and Dani Haas, senior editor, and reviewed by Jonathan Pedneault, crisis and conflict researcher; Zama Neff, children’s rights director; Brian Root, senior quantitative analyst; Kyle Knight, senior researcher on LGBT rights; Kriti Sharma, senior disability rights researcher; and Patricia Gossman, associate Asia director. James Ross, legal and policy director, provided legal review.
Production assistance was provided by Travis Carr, publications coordinator; Fitzroy Hepkins, senior administrative manager; and José Martínez, administrative officer.
Our thanks to the Afghan government for allowing us to visit government hospitals and to Dr. Najmusama Shefajo and her staff for their kind help. Huge thanks to all the healthcare workers who helped us and spoke with us and who are making a difference every day for women under extremely difficult conditions, through insecurity and with the barest of resources. We also appreciate donors and experts who spoke frankly about their concerns over declining funding. Our greatest thanks, of course, go to the women we interviewed who shared their stories with us, which were often painful, and did so during what were sometimes particularly difficult moments in their lives.
In response to the evolving situation in Afghanistan, Human Rights Watch has decided to edit visual elements of this publication temporarily for security reasons.